Portable Heart Boxes Enables Safer Transplantation
|
By HospiMedica International staff writers Posted on 23 Jun 2020 |
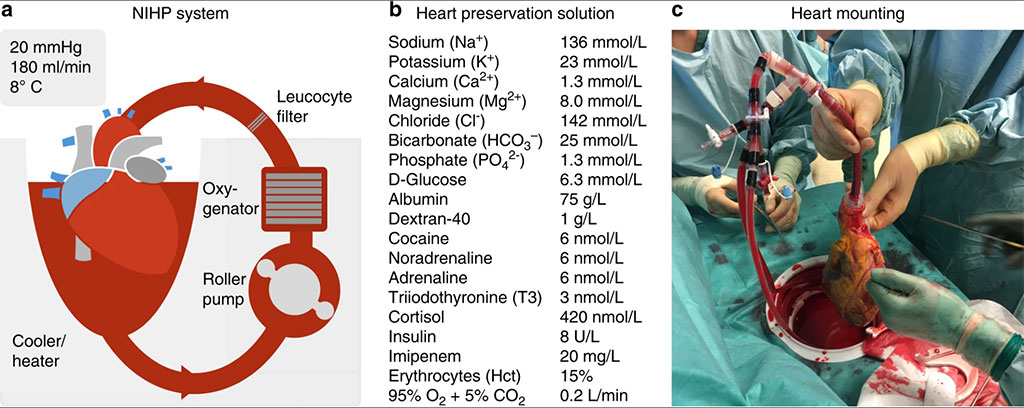
Image: Schematic of the NIHP system (Photo courtesy of Nature Communications)
A portable non-ischemic heart preservation (NIHP) device facilitates ground and airborne transportation of human hearts, according to a new study.
Researchers at Lund University (LU; Sweden) and Skåne University Hospital (Skåne; Malmö, Sweden) conducted a prospective, open-label, phase II study comparing NIHP to static cold preservation (SCS) in 31 adult recipients on waiting lists for heart transplantation; of these, six were assigned to NIHP and 25 to SCS. NIHP was scheduled in advance, based on availability of trained team members. The primary endpoint was a composite of survival free of severe primary graft dysfunction, extracorporeal membrane oxygenation (ECMO) use within seven days, and acute cellular rejection within six months.
The results showed median preservation time was 223 minutes for NIHP and 194 minutes for SCS. Over the first six months, all of the patients assigned to NIHP achieved event-free survival, compared to 18 of those assigned to SCS (72%); these included four deaths and three cardiac-related adverse events. In addition, creatine kinase myocardial band (CK-MB) level assessed six hours after ending perfusion was 76 ng/mL for NIHP, compared with 138 ng/mL for SCS. The study was published on June 12, 2020, in Nature Communications.
“Our study shows that the new method enables longer preservation than today. If we, in our continued research, can establish that this is possible, it would mean entirely new opportunities for transplants. It would, for example, be possible to fly hearts between countries, which we are currently cannot,” said lead author Professor Johan Nilsson, MD, of LU and Skåne. “Although it is too early to draw far-reaching conclusions, we are obviously hopeful. If our results continue to be positive, the method could make a big difference for patients needing a heart transplant.”
The cornerstone of organ preservation has been SCS, which is ischemic. Although SCS reduces the extent of organ damage during transport, significant deterioration of the donated organ still occurs; the longer the organ is kept on ice, the greater the damage. During NIHP, in contrast, the heart is continuously perfused with a cold (8 °C) oxygenated cardioplegic nutrition–hormone solution containing erythrocytes. It is estimated that 60-65% of donor hearts globally cannot ultimately be used for transplantation due to the limitations of cold storage.
Related Links:
Lund University
Skåne University Hospital
Researchers at Lund University (LU; Sweden) and Skåne University Hospital (Skåne; Malmö, Sweden) conducted a prospective, open-label, phase II study comparing NIHP to static cold preservation (SCS) in 31 adult recipients on waiting lists for heart transplantation; of these, six were assigned to NIHP and 25 to SCS. NIHP was scheduled in advance, based on availability of trained team members. The primary endpoint was a composite of survival free of severe primary graft dysfunction, extracorporeal membrane oxygenation (ECMO) use within seven days, and acute cellular rejection within six months.
The results showed median preservation time was 223 minutes for NIHP and 194 minutes for SCS. Over the first six months, all of the patients assigned to NIHP achieved event-free survival, compared to 18 of those assigned to SCS (72%); these included four deaths and three cardiac-related adverse events. In addition, creatine kinase myocardial band (CK-MB) level assessed six hours after ending perfusion was 76 ng/mL for NIHP, compared with 138 ng/mL for SCS. The study was published on June 12, 2020, in Nature Communications.
“Our study shows that the new method enables longer preservation than today. If we, in our continued research, can establish that this is possible, it would mean entirely new opportunities for transplants. It would, for example, be possible to fly hearts between countries, which we are currently cannot,” said lead author Professor Johan Nilsson, MD, of LU and Skåne. “Although it is too early to draw far-reaching conclusions, we are obviously hopeful. If our results continue to be positive, the method could make a big difference for patients needing a heart transplant.”
The cornerstone of organ preservation has been SCS, which is ischemic. Although SCS reduces the extent of organ damage during transport, significant deterioration of the donated organ still occurs; the longer the organ is kept on ice, the greater the damage. During NIHP, in contrast, the heart is continuously perfused with a cold (8 °C) oxygenated cardioplegic nutrition–hormone solution containing erythrocytes. It is estimated that 60-65% of donor hearts globally cannot ultimately be used for transplantation due to the limitations of cold storage.
Related Links:
Lund University
Skåne University Hospital
Latest Surgical Techniques News
- Miniaturized Implantable Multi-Sensors Device to Monitor Vessels Health
- Tiny Robots Made Out Of Carbon Could Conduct Colonoscopy, Pelvic Exam or Blood Test
- Miniaturized Ultrasonic Scalpel Enables Faster and Safer Robotic-Assisted Surgery
- AI Assisted Reading Tool for Small Bowel Video Capsule Endoscopy Detects More Lesions
- First-Ever Contact Force Pulsed Field Ablation System to Transform Treatment of Ventricular Arrhythmias
- Caterpillar Robot with Built-In Steering System Crawls Easily Through Loops and Bends
- Tiny Wraparound Electronic Implants to Revolutionize Treatment of Spinal Cord Injuries
- Small, Implantable Cardiac Pump to Help Children Awaiting Heart Transplant
- Gastrointestinal Imaging Capsule a Game-Changer in Esophagus Surveillance and Treatment
- World’s Smallest Laser Probe for Brain Procedures Facilitates Ablation of Full Range of Targets
- Artificial Intelligence Broadens Diagnostic Abilities of Conventional Coronary Angiography
- AI-Powered Surgical Visualization Tool Supports Surgeons' Visual Recognition in Real Time
- Cutting-Edge Robotic Bronchial Endoscopic System Provides Prompt Intervention during Emergencies
- Handheld Device for Fluorescence-Guided Surgery a Game Changer for Removal of High-Grade Glioma Brain Tumors
- Porous Gel Sponge Facilitates Rapid Hemostasis and Wound Healing
- Novel Rigid Endoscope System Enables Deep Tissue Imaging During Surgery
Channels
Artificial Intelligence
view channel
AI-Powered Algorithm to Revolutionize Detection of Atrial Fibrillation
Atrial fibrillation (AFib), a condition characterized by an irregular and often rapid heart rate, is linked to increased risks of stroke and heart failure. This is because the irregular heartbeat in AFib... Read more
AI Diagnostic Tool Accurately Detects Valvular Disorders Often Missed by Doctors
Doctors generally use stethoscopes to listen for the characteristic lub-dub sounds made by heart valves opening and closing. They also listen for less prominent sounds that indicate problems with these valves.... Read moreCritical Care
view channel
Powerful AI Risk Assessment Tool Predicts Outcomes in Heart Failure Patients
Heart failure is a serious condition where the heart cannot pump sufficient blood to meet the body's needs, leading to symptoms like fatigue, weakness, and swelling in the legs and feet, and it can ultimately... Read more
Peptide-Based Hydrogels Repair Damaged Organs and Tissues On-The-Spot
Scientists have ingeniously combined biomedical expertise with nature-inspired engineering to develop a jelly-like material that holds significant promise for immediate repairs to a wide variety of damaged... Read more
One-Hour Endoscopic Procedure Could Eliminate Need for Insulin for Type 2 Diabetes
Over 37 million Americans are diagnosed with diabetes, and more than 90% of these cases are Type 2 diabetes. This form of diabetes is most commonly seen in individuals over 45, though an increasing number... Read morePatient Care
view channelFirst-Of-Its-Kind Portable Germicidal Light Technology Disinfects High-Touch Clinical Surfaces in Seconds
Reducing healthcare-acquired infections (HAIs) remains a pressing issue within global healthcare systems. In the United States alone, 1.7 million patients contract HAIs annually, leading to approximately... Read more
Surgical Capacity Optimization Solution Helps Hospitals Boost OR Utilization
An innovative solution has the capability to transform surgical capacity utilization by targeting the root cause of surgical block time inefficiencies. Fujitsu Limited’s (Tokyo, Japan) Surgical Capacity... Read more
Game-Changing Innovation in Surgical Instrument Sterilization Significantly Improves OR Throughput
A groundbreaking innovation enables hospitals to significantly improve instrument processing time and throughput in operating rooms (ORs) and sterile processing departments. Turbett Surgical, Inc.... Read moreHealth IT
view channel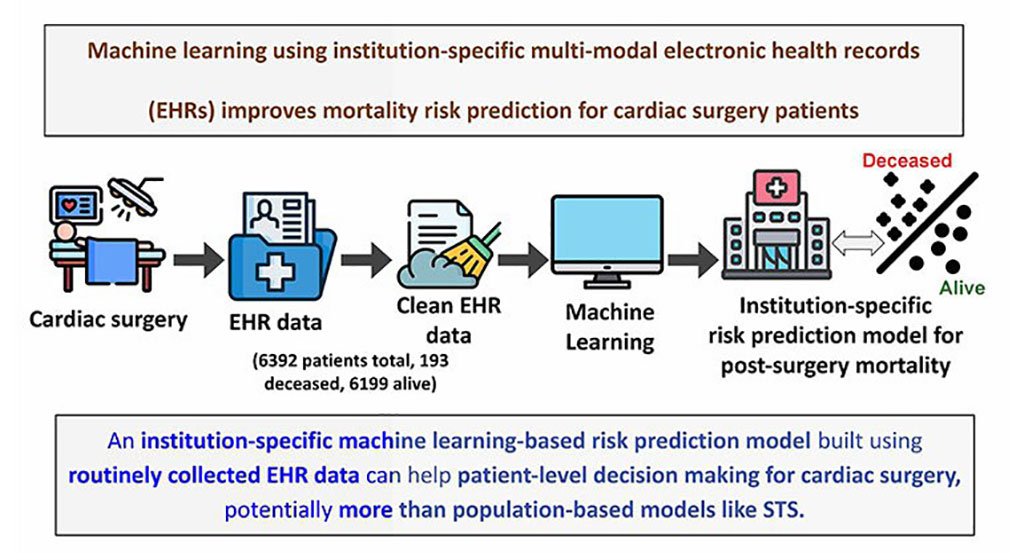
Machine Learning Model Improves Mortality Risk Prediction for Cardiac Surgery Patients
Machine learning algorithms have been deployed to create predictive models in various medical fields, with some demonstrating improved outcomes compared to their standard-of-care counterparts.... Read more
Strategic Collaboration to Develop and Integrate Generative AI into Healthcare
Top industry experts have underscored the immediate requirement for healthcare systems and hospitals to respond to severe cost and margin pressures. Close to half of U.S. hospitals ended 2022 in the red... Read more
AI-Enabled Operating Rooms Solution Helps Hospitals Maximize Utilization and Unlock Capacity
For healthcare organizations, optimizing operating room (OR) utilization during prime time hours is a complex challenge. Surgeons and clinics face difficulties in finding available slots for booking cases,... Read more
AI Predicts Pancreatic Cancer Three Years before Diagnosis from Patients’ Medical Records
Screening for common cancers like breast, cervix, and prostate cancer relies on relatively simple and highly effective techniques, such as mammograms, Pap smears, and blood tests. These methods have revolutionized... Read morePoint of Care
view channel
Critical Bleeding Management System to Help Hospitals Further Standardize Viscoelastic Testing
Surgical procedures are often accompanied by significant blood loss and the subsequent high likelihood of the need for allogeneic blood transfusions. These transfusions, while critical, are linked to various... Read more
Point of Care HIV Test Enables Early Infection Diagnosis for Infants
Early diagnosis and initiation of treatment are crucial for the survival of infants infected with HIV (human immunodeficiency virus). Without treatment, approximately 50% of infants who acquire HIV during... Read more
Whole Blood Rapid Test Aids Assessment of Concussion at Patient's Bedside
In the United States annually, approximately five million individuals seek emergency department care for traumatic brain injuries (TBIs), yet over half of those suspecting a concussion may never get it checked.... Read more
New Generation Glucose Hospital Meter System Ensures Accurate, Interference-Free and Safe Use
A new generation glucose hospital meter system now comes with several features that make hospital glucose testing easier and more secure while continuing to offer accuracy, freedom from interference, and... Read moreBusiness
view channel
Johnson & Johnson Acquires Cardiovascular Medical Device Company Shockwave Medical
Johnson & Johnson (New Brunswick, N.J., USA) and Shockwave Medical (Santa Clara, CA, USA) have entered into a definitive agreement under which Johnson & Johnson will acquire all of Shockwave’s... Read more