3D-Printed Scaffolds Reconstruct Craniofacial Defects
|
By HospiMedica International staff writers Posted on 03 Apr 2018 |

Image: Dr. Venu Varanasi and Research Assistant Tugba Cebe set the coordinates for the 3D printer (Photo courtesy of TAMU).
In-situ three-dimensional (3D) printing of osteogenic (bone regenerating) scaffolds can be used for the proper and rapid healing of bone fractures, claims a new study.
Developed by researchers at Texas A&M University (TAMU; College Station, TX, USA), the University of Texas (Arlington, USA), and other institutions, the substrate ink for the biosilica-biopolymer scaffold was prepared by mixing Laponite (Lp) with methacrylated gelatin (MAG); sucrose was used to increase viscosity and reduce gelation of the printing ink. During additive printing, crosslinking was initiated by ultra-violet (UV) light at the tip of the printer nozzle and, and the scaffolds were 3D printed in-situ, directly into calvaria bone defects using varied Laponite concentration so as to determine optimal bone density and chemical structure.
The scaffolds were fabricated into a mesh design, with dimensions matching that of formed defects; after four weeks, cranial bone samples were extracted. Evaluation by micro-CT showed that nearly 55% of the bone defect was healed for higher Lp- rich-MAG scaffolds, whereas empty control defects only had 11% of the defect filled with bone after four weeks. Histological staining showed that the scaffolds recruited osteoblasts and blood and growth factors into their structure to regenerate the intra-bony layers needed to initiate the healing process. The study was presented at the International & American Associations for Dental Research annual meeting, held during March 2018 in Fort Lauderdale (FL, USA).
“The results showed that 3D in-situ printing of bone regenerating scaffolds did improve the delivery of regenerative and reconstructive biomedical devices for the proper and rapid healing of bone fractures,” said senior author and study presenter Venu Varanasi, PhD, of TAMU. “This provides an advantage in that cells from within the initial hematoma become incorporated into the scaffold structure, thus, giving the operator flexibility to use the printed scaffold as a structural support that stimulates healing.”
“The gold standard for reconstruction of craniofacial defects involves carving of the cranial bone, hip bone, or the leg bone to recreate the missing structures. This is technically impossible for large facial defects,” said maxillofacial surgeon Likith Reddy, DDS, MD, director of residency training at the TAMU School of Dentistry. “If the technology works as anticipated, it will revolutionize the reconstruction of such complex three-dimensional structures. Reconstruction of such complex facial bony defects would become less of an art and more of a science.”
Severe traumatic injuries to the cranium have been challenging to heal due to the large missing bone volume. Typically, metal or plastic implants are used. But, these implants can take a long time to be customized for fit and often take a longer than desired time to support bone fixation. This can often lead to multiple revision surgeries if the defect is not properly healed. Moreover, the tissue that adjoins the implant can improperly heal.
Related Links:
Texas A&M University
University of Texas
Developed by researchers at Texas A&M University (TAMU; College Station, TX, USA), the University of Texas (Arlington, USA), and other institutions, the substrate ink for the biosilica-biopolymer scaffold was prepared by mixing Laponite (Lp) with methacrylated gelatin (MAG); sucrose was used to increase viscosity and reduce gelation of the printing ink. During additive printing, crosslinking was initiated by ultra-violet (UV) light at the tip of the printer nozzle and, and the scaffolds were 3D printed in-situ, directly into calvaria bone defects using varied Laponite concentration so as to determine optimal bone density and chemical structure.
The scaffolds were fabricated into a mesh design, with dimensions matching that of formed defects; after four weeks, cranial bone samples were extracted. Evaluation by micro-CT showed that nearly 55% of the bone defect was healed for higher Lp- rich-MAG scaffolds, whereas empty control defects only had 11% of the defect filled with bone after four weeks. Histological staining showed that the scaffolds recruited osteoblasts and blood and growth factors into their structure to regenerate the intra-bony layers needed to initiate the healing process. The study was presented at the International & American Associations for Dental Research annual meeting, held during March 2018 in Fort Lauderdale (FL, USA).
“The results showed that 3D in-situ printing of bone regenerating scaffolds did improve the delivery of regenerative and reconstructive biomedical devices for the proper and rapid healing of bone fractures,” said senior author and study presenter Venu Varanasi, PhD, of TAMU. “This provides an advantage in that cells from within the initial hematoma become incorporated into the scaffold structure, thus, giving the operator flexibility to use the printed scaffold as a structural support that stimulates healing.”
“The gold standard for reconstruction of craniofacial defects involves carving of the cranial bone, hip bone, or the leg bone to recreate the missing structures. This is technically impossible for large facial defects,” said maxillofacial surgeon Likith Reddy, DDS, MD, director of residency training at the TAMU School of Dentistry. “If the technology works as anticipated, it will revolutionize the reconstruction of such complex three-dimensional structures. Reconstruction of such complex facial bony defects would become less of an art and more of a science.”
Severe traumatic injuries to the cranium have been challenging to heal due to the large missing bone volume. Typically, metal or plastic implants are used. But, these implants can take a long time to be customized for fit and often take a longer than desired time to support bone fixation. This can often lead to multiple revision surgeries if the defect is not properly healed. Moreover, the tissue that adjoins the implant can improperly heal.
Related Links:
Texas A&M University
University of Texas
Latest Health IT News
- Machine Learning Model Improves Mortality Risk Prediction for Cardiac Surgery Patients
- Strategic Collaboration to Develop and Integrate Generative AI into Healthcare
- AI-Enabled Operating Rooms Solution Helps Hospitals Maximize Utilization and Unlock Capacity
- AI Predicts Pancreatic Cancer Three Years before Diagnosis from Patients’ Medical Records
- First Fully Autonomous Generative AI Personalized Medical Authorizations System Reduces Care Delay
- Electronic Health Records May Be Key to Improving Patient Care, Study Finds
- AI Trained for Specific Vocal Biomarkers Could Accurately Predict Coronary Artery Disease
- First-Ever AI Test for Early Diagnosis of Alzheimer’s to Be Expanded to Diagnosis of Parkinson’s Disease
- New Self-Learning AI-Based Algorithm Reads Electrocardiograms to Spot Unseen Signs of Heart Failure
- Autonomous Robot Performs COVID-19 Nasal Swab Tests

- Statistical Tool Predicts COVID-19 Peaks Worldwide
- Wireless-Controlled Soft Neural Implant Stimulates Brain Cells
- Tiny Polymer Stent Could Treat Pediatric Urethral Strictures
- Human Torso Simulator Helps Design Brace Innovations
- 3D Bioprinting Rebuilds the Human Heart
Channels
Artificial Intelligence
view channel
AI-Powered Algorithm to Revolutionize Detection of Atrial Fibrillation
Atrial fibrillation (AFib), a condition characterized by an irregular and often rapid heart rate, is linked to increased risks of stroke and heart failure. This is because the irregular heartbeat in AFib... Read more
AI Diagnostic Tool Accurately Detects Valvular Disorders Often Missed by Doctors
Doctors generally use stethoscopes to listen for the characteristic lub-dub sounds made by heart valves opening and closing. They also listen for less prominent sounds that indicate problems with these valves.... Read moreCritical Care
view channel
Stretchable Microneedles to Help In Accurate Tracking of Abnormalities and Identifying Rapid Treatment
The field of personalized medicine is transforming rapidly, with advancements like wearable devices and home testing kits making it increasingly easy to monitor a wide range of health metrics, from heart... Read more
Machine Learning Tool Identifies Rare, Undiagnosed Immune Disorders from Patient EHRs
Patients suffering from rare diseases often endure extensive delays in receiving accurate diagnoses and treatments, which can lead to unnecessary tests, worsening health, psychological strain, and significant... Read more
On-Skin Wearable Bioelectronic Device Paves Way for Intelligent Implants
A team of researchers at the University of Missouri (Columbia, MO, USA) has achieved a milestone in developing a state-of-the-art on-skin wearable bioelectronic device. This development comes from a lab... Read more
First-Of-Its-Kind Dissolvable Stent to Improve Outcomes for Patients with Severe PAD
Peripheral artery disease (PAD) affects millions and presents serious health risks, particularly its severe form, chronic limb-threatening ischemia (CLTI). CLTI develops when arteries are blocked by plaque,... Read moreSurgical Techniques
view channel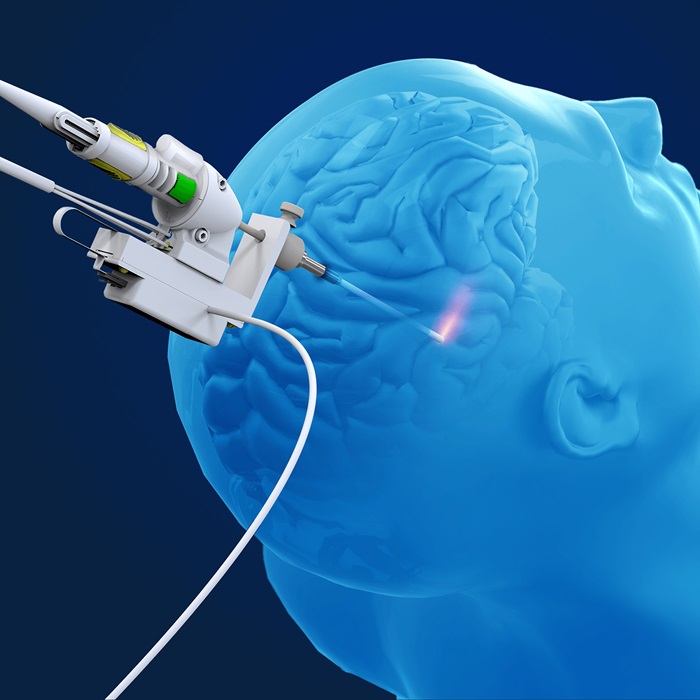
World’s Smallest Laser Probe for Brain Procedures Facilitates Ablation of Full Range of Targets
A new probe enhances the ablation capabilities for a broad spectrum of oncology and epilepsy targets, including pediatric applications, by incorporating advanced laser and cooling technologies to support... Read more.jpg)
Artificial Intelligence Broadens Diagnostic Abilities of Conventional Coronary Angiography
Coronary angiography is an essential diagnostic tool used globally to identify coronary artery disease (CAD), with millions of procedures conducted annually. Traditionally, data from coronary angiograms... Read moreAI-Powered Surgical Visualization Tool Supports Surgeons' Visual Recognition in Real Time
Connective tissue serves as an essential landmark in surgical navigation, often referred to as the "dissection plane" or "holy plane." Its accurate identification is vital for achieving safe and effective... Read moreHandheld Device for Fluorescence-Guided Surgery a Game Changer for Removal of High-Grade Glioma Brain Tumors
Grade III or IV gliomas are among the most common and deadly brain tumors, with around 20,000 cases annually in the U.S. and 1.2 million globally. These tumors are very aggressive and tend to infiltrate... Read morePatient Care
view channelFirst-Of-Its-Kind Portable Germicidal Light Technology Disinfects High-Touch Clinical Surfaces in Seconds
Reducing healthcare-acquired infections (HAIs) remains a pressing issue within global healthcare systems. In the United States alone, 1.7 million patients contract HAIs annually, leading to approximately... Read more
Surgical Capacity Optimization Solution Helps Hospitals Boost OR Utilization
An innovative solution has the capability to transform surgical capacity utilization by targeting the root cause of surgical block time inefficiencies. Fujitsu Limited’s (Tokyo, Japan) Surgical Capacity... Read more
Game-Changing Innovation in Surgical Instrument Sterilization Significantly Improves OR Throughput
A groundbreaking innovation enables hospitals to significantly improve instrument processing time and throughput in operating rooms (ORs) and sterile processing departments. Turbett Surgical, Inc.... Read morePoint of Care
view channel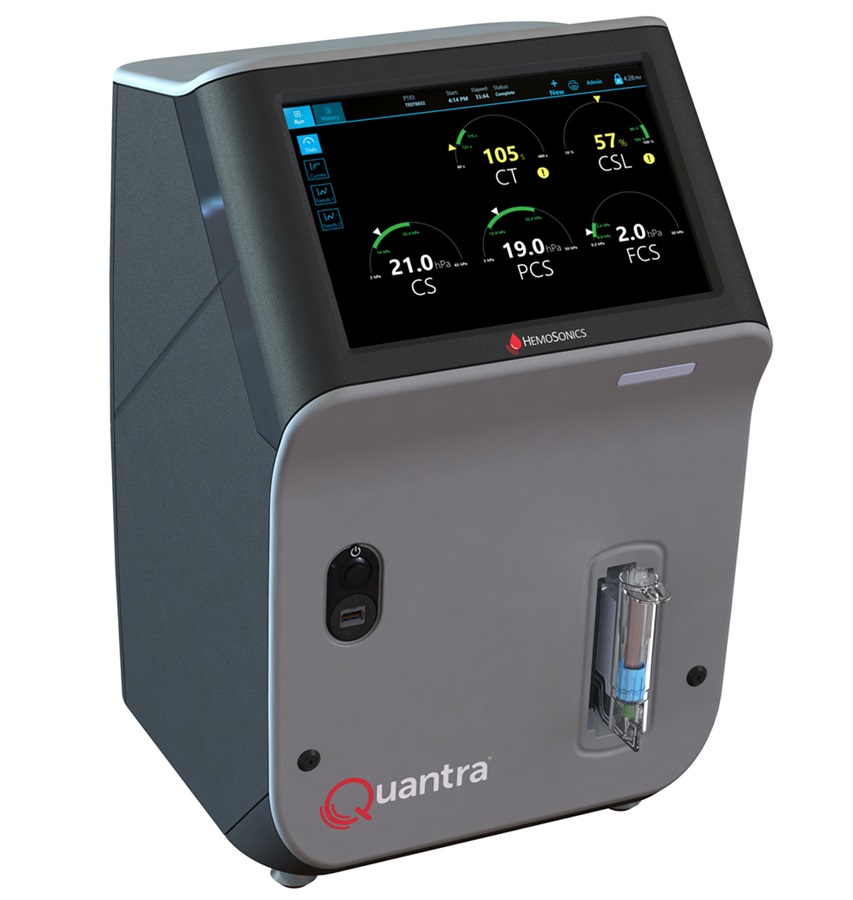
Critical Bleeding Management System to Help Hospitals Further Standardize Viscoelastic Testing
Surgical procedures are often accompanied by significant blood loss and the subsequent high likelihood of the need for allogeneic blood transfusions. These transfusions, while critical, are linked to various... Read more
Point of Care HIV Test Enables Early Infection Diagnosis for Infants
Early diagnosis and initiation of treatment are crucial for the survival of infants infected with HIV (human immunodeficiency virus). Without treatment, approximately 50% of infants who acquire HIV during... Read more
Whole Blood Rapid Test Aids Assessment of Concussion at Patient's Bedside
In the United States annually, approximately five million individuals seek emergency department care for traumatic brain injuries (TBIs), yet over half of those suspecting a concussion may never get it checked.... Read more
New Generation Glucose Hospital Meter System Ensures Accurate, Interference-Free and Safe Use
A new generation glucose hospital meter system now comes with several features that make hospital glucose testing easier and more secure while continuing to offer accuracy, freedom from interference, and... Read moreBusiness
view channel
Johnson & Johnson Acquires Cardiovascular Medical Device Company Shockwave Medical
Johnson & Johnson (New Brunswick, N.J., USA) and Shockwave Medical (Santa Clara, CA, USA) have entered into a definitive agreement under which Johnson & Johnson will acquire all of Shockwave’s... Read more