Research Recommends Elderly Patients Stop Cancer Screening
|
By HospiMedica International staff writers Posted on 06 Sep 2019 |
Despite current clinical guidelines recommend against screening older adults with less than 10 years' life expectancy, many doctors continue to do so, claims a new study.
The study, by researchers at Johns Hopkins University School of Medicine (JHU-SOM; Baltimore, MD, USA) and the University of California, San Francisco (UCSF; USA), examined the perspectives of both clinicians and older adults on how to communicate about stopping cancer screening. To do so, they interviewed 28 clinicians (including physicians, certified registered nurse practitioners and physician assistants) and 40 older adults (65-92 years of age, 57.5% female, 62.5% white) on their viewpoints on cancer screening discussions. All interviews were audio-recorded and transcribed.
The results revealed that both clinicians and patients thought it was important to frame discussions around stopping cancer screening in terms of risks and benefits. While screening can reveal tumors, it can also lead to complications from screening--such as colon perforations during a colonoscopy--and to risks and side effects from follow-up tests and treatment, such as the infection, fatigue, and bleeding associated with chemotherapy. Cancer diagnosis may also lead to diverted attention from other health priorities, increased psychological stress and a financial burden on patients.
The patients and clinicians also agreed that patients should play an active role in making the decision to stop screening, as clinicians tended to worry that patients might perceive the recommendation to stop screening in a negative light and that it would make patients angry. However, most patients responded that if they trusted their clinician, initiating the conversation would not be perceived in a negative light. And while clinicians almost unanimously reported that they did not raise life expectancy in the context of stopping cancer screening, older adults were divided on the issue, with some wanting to hear about it and others actively against it. The study was published in the June 2019 issue of The Gerontologist.
“Given the heterogeneity in older adults’ preferences, it is important to assess whether patients want to discuss life expectancy when discussing stopping cancer screening, though use of the specific term ‘life expectancy’ may not be necessary,” said lead author Nancy Schoenborn, MD, of JHU-SOM. “Instead, focusing discussion on the benefits and risks of cancer screening and mentioning shift in health priorities are acceptable communication strategies for both clinicians and older adults.”
One example of this issue is adenoma surveillance. The cut off age for stopping surveillance is usually quoted as 75 years, as the remaining life expectancy is likely less than the average time required for new adenomas to become malignant. After 75, it is unlikely that the benefits of surveillance will outweigh the potential risks of the procedure.
Related Links:
Johns Hopkins University School of Medicine
University of California, San Francisco
The study, by researchers at Johns Hopkins University School of Medicine (JHU-SOM; Baltimore, MD, USA) and the University of California, San Francisco (UCSF; USA), examined the perspectives of both clinicians and older adults on how to communicate about stopping cancer screening. To do so, they interviewed 28 clinicians (including physicians, certified registered nurse practitioners and physician assistants) and 40 older adults (65-92 years of age, 57.5% female, 62.5% white) on their viewpoints on cancer screening discussions. All interviews were audio-recorded and transcribed.
The results revealed that both clinicians and patients thought it was important to frame discussions around stopping cancer screening in terms of risks and benefits. While screening can reveal tumors, it can also lead to complications from screening--such as colon perforations during a colonoscopy--and to risks and side effects from follow-up tests and treatment, such as the infection, fatigue, and bleeding associated with chemotherapy. Cancer diagnosis may also lead to diverted attention from other health priorities, increased psychological stress and a financial burden on patients.
The patients and clinicians also agreed that patients should play an active role in making the decision to stop screening, as clinicians tended to worry that patients might perceive the recommendation to stop screening in a negative light and that it would make patients angry. However, most patients responded that if they trusted their clinician, initiating the conversation would not be perceived in a negative light. And while clinicians almost unanimously reported that they did not raise life expectancy in the context of stopping cancer screening, older adults were divided on the issue, with some wanting to hear about it and others actively against it. The study was published in the June 2019 issue of The Gerontologist.
“Given the heterogeneity in older adults’ preferences, it is important to assess whether patients want to discuss life expectancy when discussing stopping cancer screening, though use of the specific term ‘life expectancy’ may not be necessary,” said lead author Nancy Schoenborn, MD, of JHU-SOM. “Instead, focusing discussion on the benefits and risks of cancer screening and mentioning shift in health priorities are acceptable communication strategies for both clinicians and older adults.”
One example of this issue is adenoma surveillance. The cut off age for stopping surveillance is usually quoted as 75 years, as the remaining life expectancy is likely less than the average time required for new adenomas to become malignant. After 75, it is unlikely that the benefits of surveillance will outweigh the potential risks of the procedure.
Related Links:
Johns Hopkins University School of Medicine
University of California, San Francisco
Latest Patient Care News
- Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
- Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
- VR Training Tool Combats Contamination of Portable Medical Equipment
- Portable Biosensor Platform to Reduce Hospital-Acquired Infections
- First-Of-Its-Kind Portable Germicidal Light Technology Disinfects High-Touch Clinical Surfaces in Seconds
- Surgical Capacity Optimization Solution Helps Hospitals Boost OR Utilization

- Game-Changing Innovation in Surgical Instrument Sterilization Significantly Improves OR Throughput
- Next Gen ICU Bed to Help Address Complex Critical Care Needs
- Groundbreaking AI-Powered UV-C Disinfection Technology Redefines Infection Control Landscape
- Clean Hospitals Can Reduce Antibiotic Resistance, Save Lives
- Smart Hospital Beds Improve Accuracy of Medical Diagnosis
- New Fast Endoscope Drying System Improves Productivity and Traceability
- World’s First Automated Endoscope Cleaner Fights Antimicrobial Resistance
- Portable High-Capacity Digital Stretcher Scales Provide Precision Weighing for Patients in ER
- Portable Clinical Scale with Remote Indicator Allows for Flexible Patient Weighing Use
- Innovative and Highly Customizable Medical Carts Offer Unlimited Configuration Possibilities
Channels
Artificial Intelligence
view channelAI Analysis of Pericardial Fat Refines Long-Term Heart Disease Risk
Accurately identifying long-term cardiovascular disease risk in asymptomatic adults remains challenging for clinicians. Missed or underestimated risk delays preventive therapy and increases the chance... Read more
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read moreCritical Care
view channel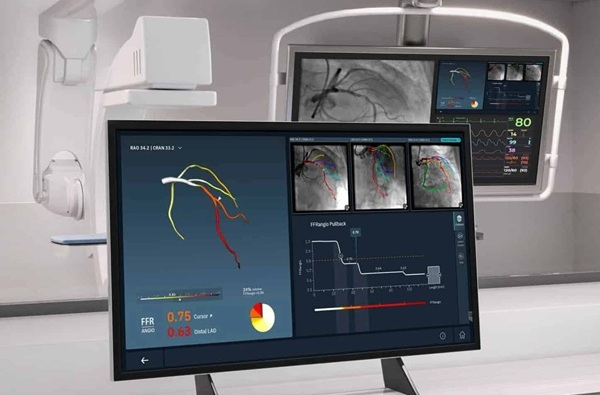
Angiography-Based FFR Approach Matches Gold Standard Results Without Wires
Accurately determining whether a coronary stenosis limits blood flow is essential to guide percutaneous coronary intervention, yet wire-based physiologic testing remains underused due to added procedural... Read more
Eye Imaging AI Identifies Elevated Cardiovascular Risk
Many adults at risk for atherosclerotic cardiovascular disease are not identified until they undergo formal primary care assessment. Delayed risk recognition can postpone initiation of statins and lifestyle... Read moreSurgical Techniques
view channel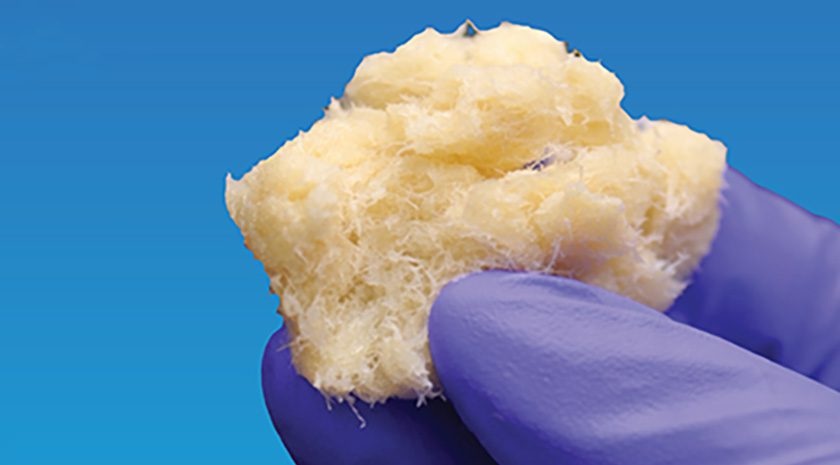
Fiber-Form Bone Graft Expands Intraoperative Options for Spinal Fusion
Spinal and orthopedic fusion procedures often require bone graft materials that handle predictably and support bone formation. Surgeons face added complexity in difficult anatomy and challenging fusion environments.... Read more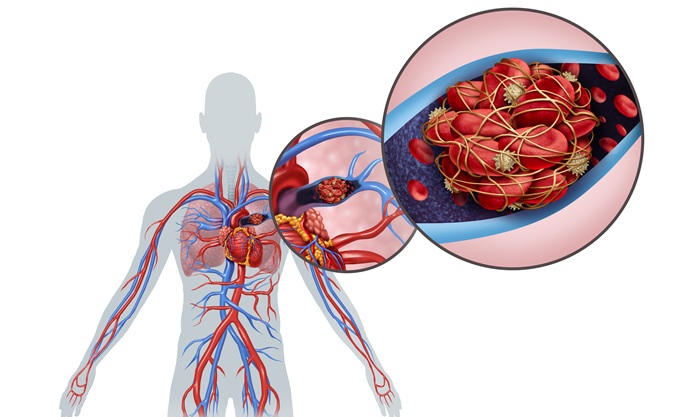
Ultrasound‑Aided Catheter Treatment Cuts Early Collapse in Pulmonary Embolism
Acute pulmonary embolism can cause rapid hemodynamic deterioration and early death in hospitalized and emergency patients. Systemic thrombolysis can dissolve clots but is limited by a high risk of major... Read moreHealth IT
view channel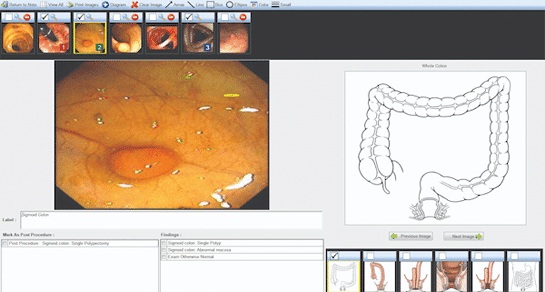
Voice-Driven AI System Enables Structured GI Procedure Documentation
Documentation during gastrointestinal (GI) procedures often competes with real-time clinical decision-making and imposes a significant cognitive burden on physicians. Manual data entry and post-procedure... Read more
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel




















