Home-Based System Relieves Cirrhosis Refractory Ascites
|
By HospiMedica International staff writers Posted on 11 Jan 2022 |
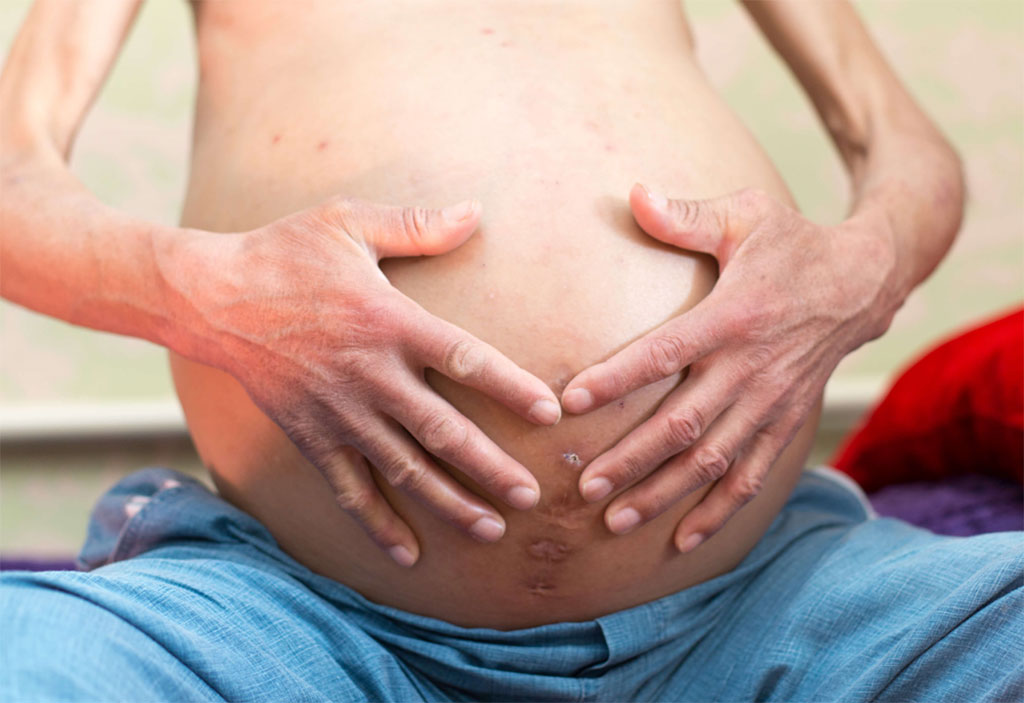
Image: An ascites patient with abdominal paracentesis scars (Photo courtesy of iStock)
A novel tunneled peritoneal catheter (PeCa) drainage system provided significant relief for patients with refractory ascites, according to a new study.
The PeCa implant, developed at Hannover Medical School (Germany), is composed of internal shut that lies in the peritoneal cavity, a tunneled section that passes through subcutaneous tissue, and an external port to which drainage bags are connected. To test system efficacy, outcomes in 152 patients with refractory ascites, who were not candidates for transjugular intrahepatic portosystemic shunt (TIPS) and received a PeCa implant, were compared to 71 patients who received standard care, which included repeated large volume paracentesis and albumin.
The results revealed that factors associated with 90-day survival were PeCa implantation, and each point of Model for End-Stage Liver Disease (MELD) score. Hospitalizations were more common in the PeCa group, for reasons that included spontaneous bacterial peritonitis (SBP), hyponatremia, and infections other than SBP. There was no significant difference in mortality between the two groups, but there were trends in the PeCa group towards higher frequency of acute kidney injury (AKI). The study was presented at the American Association for the Study of Liver Diseases annual conference, held online during November 2021.
“Patients with refractory ascites have a very high risk for rehospitalization, AKI, and death. Our data indicate that PeCa could be a valuable new treatment option for patients with refractory ascites and contraindication for TIPS,” said study co-author and presenter Tammo Lambert Tergast, MD. “I think if we can optimize the treatment after discharge, we can also minimize the rehospitalization in these patients. However, the risk for hyponatremia and AKI has to be considered and further explored.”
Refractory ascites occurs when patients no longer respond to medical therapy, a condition that affects over 100,000 patients in Europe and the United States every year, a number that is growing at approximately 10% a year. The primary treatment for ascites is paracentesis, a procedure in which a large bore needle is inserted into the patient's abdomen to remove between 5‐10 liters of ascites that has accumulated over a period of a week or two.
Related Links:
Hannover Medical School
The PeCa implant, developed at Hannover Medical School (Germany), is composed of internal shut that lies in the peritoneal cavity, a tunneled section that passes through subcutaneous tissue, and an external port to which drainage bags are connected. To test system efficacy, outcomes in 152 patients with refractory ascites, who were not candidates for transjugular intrahepatic portosystemic shunt (TIPS) and received a PeCa implant, were compared to 71 patients who received standard care, which included repeated large volume paracentesis and albumin.
The results revealed that factors associated with 90-day survival were PeCa implantation, and each point of Model for End-Stage Liver Disease (MELD) score. Hospitalizations were more common in the PeCa group, for reasons that included spontaneous bacterial peritonitis (SBP), hyponatremia, and infections other than SBP. There was no significant difference in mortality between the two groups, but there were trends in the PeCa group towards higher frequency of acute kidney injury (AKI). The study was presented at the American Association for the Study of Liver Diseases annual conference, held online during November 2021.
“Patients with refractory ascites have a very high risk for rehospitalization, AKI, and death. Our data indicate that PeCa could be a valuable new treatment option for patients with refractory ascites and contraindication for TIPS,” said study co-author and presenter Tammo Lambert Tergast, MD. “I think if we can optimize the treatment after discharge, we can also minimize the rehospitalization in these patients. However, the risk for hyponatremia and AKI has to be considered and further explored.”
Refractory ascites occurs when patients no longer respond to medical therapy, a condition that affects over 100,000 patients in Europe and the United States every year, a number that is growing at approximately 10% a year. The primary treatment for ascites is paracentesis, a procedure in which a large bore needle is inserted into the patient's abdomen to remove between 5‐10 liters of ascites that has accumulated over a period of a week or two.
Related Links:
Hannover Medical School
Latest Patient Care News
- AI Avatar Doctor Improves Patient Understanding Before Radiotherapy
- Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
- Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
- VR Training Tool Combats Contamination of Portable Medical Equipment
- Portable Biosensor Platform to Reduce Hospital-Acquired Infections
- First-Of-Its-Kind Portable Germicidal Light Technology Disinfects High-Touch Clinical Surfaces in Seconds
- Surgical Capacity Optimization Solution Helps Hospitals Boost OR Utilization

- Game-Changing Innovation in Surgical Instrument Sterilization Significantly Improves OR Throughput
- Next Gen ICU Bed to Help Address Complex Critical Care Needs
- Groundbreaking AI-Powered UV-C Disinfection Technology Redefines Infection Control Landscape
- Clean Hospitals Can Reduce Antibiotic Resistance, Save Lives
- Smart Hospital Beds Improve Accuracy of Medical Diagnosis
- New Fast Endoscope Drying System Improves Productivity and Traceability
- World’s First Automated Endoscope Cleaner Fights Antimicrobial Resistance
- Portable High-Capacity Digital Stretcher Scales Provide Precision Weighing for Patients in ER
- Portable Clinical Scale with Remote Indicator Allows for Flexible Patient Weighing Use
Channels
Artificial Intelligence
view channel
AI Platform Supports Noninvasive Remote Hemodynamic Monitoring in Heart Failure
Heart failure remains a leading cause of hospitalization in adults over 65, affecting more than 6.7 million people in the U.S. Clinicians often lose visibility into hemodynamic deterioration once patients... Read more
AI Tool Predicts Unplanned Care and Symptom Burden in Cancer Survivors
Unplanned emergency visits and hospitalizations remain common in cancer survivorship, when routine clinical contact often tapers while new symptoms emerge. These events reflect unmet needs and disrupt... Read moreCritical Care
view channel
Smartphone Heart Rhythm App Reduces Unnecessary Cardioversion Procedures
Atrial fibrillation, an irregular and often rapid heart rhythm, is the most common arrhythmia in adults. Elective electrical cardioversion is frequently canceled on the day of treatment when patients revert... Read more
New Practice Guidance Supports Prostatic Artery Embolization for BPH Symptoms
Benign prostatic hyperplasia is a noncancerous enlargement of the prostate that can cause lower urinary tract symptoms and impair daily functioning. These symptoms erode sleep, productivity, and sexual... Read more
Bedside CSF Monitor Detects Early Infection in Fluid Drains
External drainage of cerebrospinal fluid (CSF) after traumatic brain injury, hydrocephalus, or hemorrhage carries a significant risk of infection. These infections can prolong intensive care, cause severe... Read more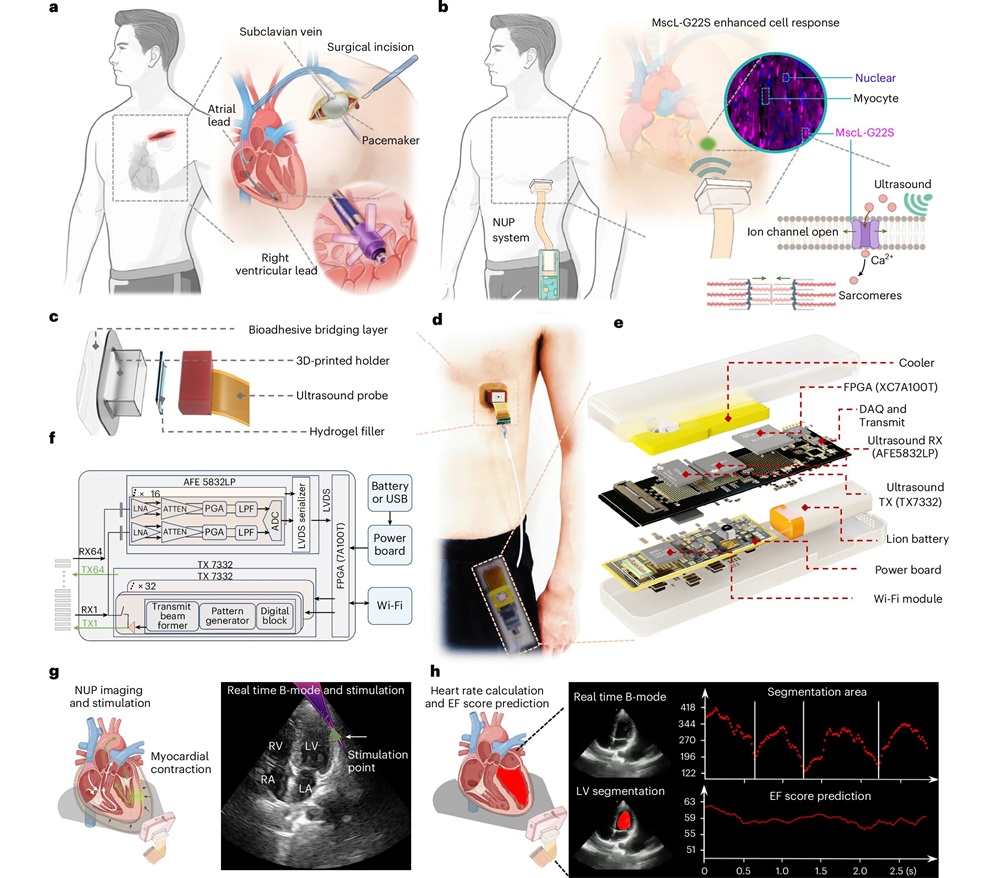
Wearable Ultrasound Patch Noninvasively Paces Heart to Stabilize Arrhythmias
Cardiac arrhythmias, including slow and irregular heart rhythms, often require pacemakers that are surgically implanted. While effective, implants carry procedural risks and long-term device maintenance burdens.... Read moreSurgical Techniques
view channel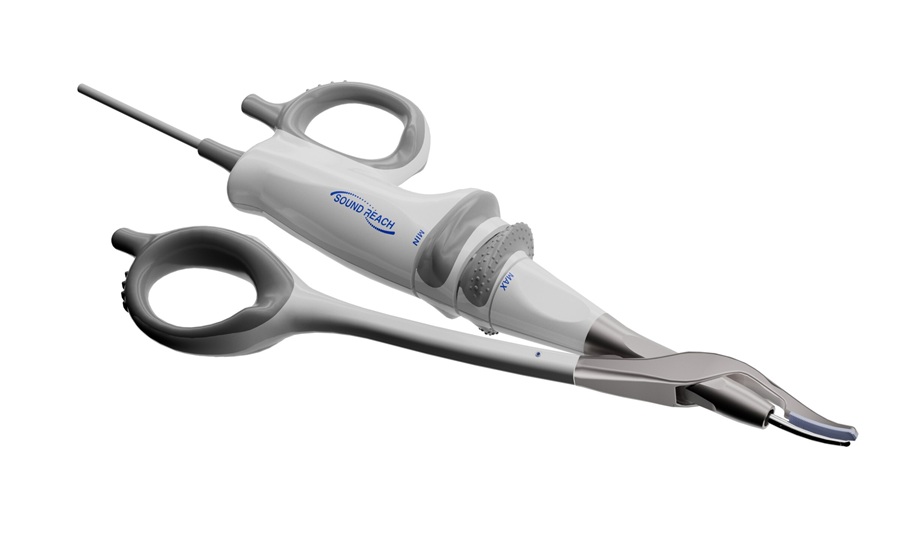
CE-Marked Ultrasonic Shears Streamline Breast and Thyroid Surgery
Thyroid and breast surgeries are often performed in confined anatomical spaces near critical structures, making precise dissection and controlled thermal management essential. As the global disease burden... Read more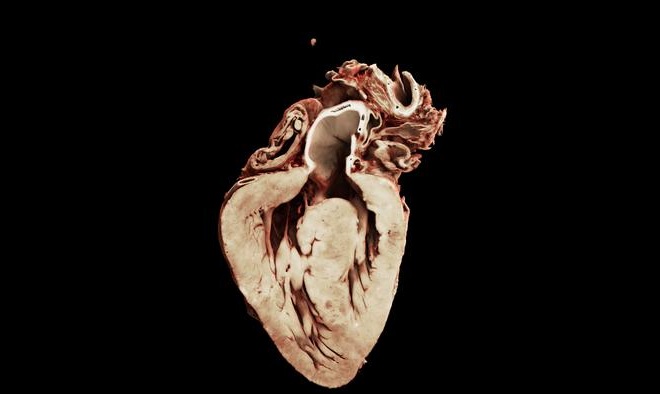
3D Map of Heart Electrical Wiring Aims to Guide Congenital Heart Repair
Tetralogy of Fallot is one of the most common congenital heart problems and often requires surgery in infancy. Many survivors later develop conduction abnormalities because the cardiac electrical system... Read moreHealth IT
view channel
AI-Native EHR Achieves EU Medical Device Certification
InterSystems (Boston, MA, USA) announced that its IntelliCare electronic health record (EHR) solutions have been certified as Class IIa medical devices under the European Union Medical Device Regulation... Read more
EHR-Integrated Screening Workflow Detects Cognitive Impairment at Admission
Cognitive impairment involves difficulties with thinking, learning, memory, and decision-making, and is more common in older adults. In U.S. hospitals, more than 40% of admitted older adults have dementia,... Read morePoint of Care
view channel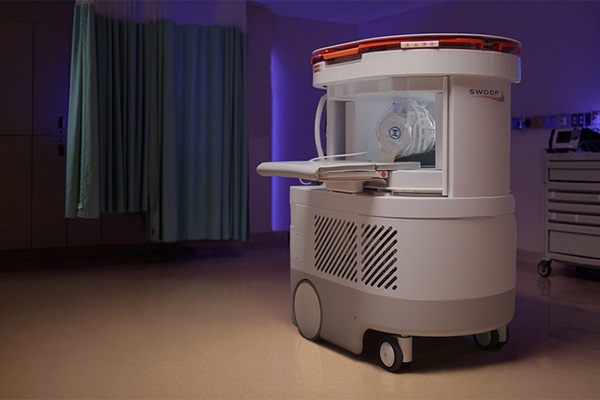
Portable MRI System Accelerates Emergency Brain Imaging and Triage
Emergency departments frequently face delays accessing conventional magnetic resonance imaging (MRI) for patients with suspected neurological emergencies. Such waits can slow triage, prolong boarding,... Read more