Eli Lilly and Incyte’s Baricitinib Receives FDA EUA for Use as Monotherapy in Hospitalized COVID-19 Patients Requiring Oxygen
|
By HospiMedica International staff writers Posted on 30 Jul 2021 |
Image: Baricitinib (Photo courtesy of Eli Lilly and Company)
The US Food and Drug Administration (FDA) has broadened the emergency use authorization (EUA) for baricitinib, a JAK1/JAK2 inhibitor licensed to Eli Lilly and Company (Indianapolis, Ind, USA) from Incyte (Wilmington, DE, USA), to allow for treatment with or without Gilead Sciences’ (Foster City, CA, USA) antiviral drug remdesivir.
The EUA was previously restricted to use only in combination with remdesivir and now provides for the use of baricitinib for treatment of COVID-19 in hospitalized adults and pediatric patients two years of age or older requiring supplemental oxygen, non-invasive or invasive mechanical ventilation or extracorporeal membrane oxygenation (ECMO). Baricitinib is a janus kinase inhibitor, which blocks the activity of one or more of a specific family of enzymes, interfering with the pathway that leads to inflammation. Baricitinib is a prescription oral tablet medication that is FDA-approved (and sold under the brand name Olumiant) for the treatment of moderately to severely active rheumatoid arthritis.
The FDA based its decision on data from the Phase 3 COV-BARRIER randomized, double-blind, placebo-controlled study of hospitalized patients comparing baricitinib 4 mg once daily plus standard of care versus placebo plus standard of care. Patients could remain on background standard of care, as defined per local guidelines, including antimalarials, antivirals, corticosteroids, and/or azithromycin. The most frequently used therapies were corticosteroids (79% of patients, mostly dexamethasone) and remdesivir (19% of patients). While the composite primary endpoint of COV-BARRIER, which was defined as a difference in the estimated proportion of participants progressing to non-invasive ventilation including high flow oxygen or invasive mechanical ventilation (including ECMO) or death by Day 28, did not meet statistical significance, baricitinib-treated patients (27.8%) were less likely than those receiving standard of care (30.5%) to progress to ventilation or death. A pre-specified key secondary endpoint showed baricitinib, in addition to standard of care, meaningfully reduced the risk of death by 39 percent by Day 28 when compared to standard of care alone.
The initial EUA was based on data from the Adaptive COVID-19 Treatment Trial (ACTT-2), a randomized double-blind, placebo-controlled study to evaluate the efficacy and safety of baricitinib in combination with remdesivir versus placebo with remdesivir in hospitalized patients with or without oxygen requirements conducted by the National Institute of Allergy and Infectious Diseases (NIAID), part of the National Institutes of Health (NIH). Data supporting the initial EUA included the primary endpoint of median time to recovery, which was seven days for baricitinib plus remdesivir compared to eight days for placebo plus remdesivir. Secondary endpoints included the proportion of patients who died or progressed to non-invasive ventilation/high-flow oxygen or invasive mechanical ventilation by Day 29, which was lower in baricitinib plus remdesivir (23%) compared to placebo plus remdesivir (28%), and the proportion of patients who died by Day 29 was 4.7% (24/515) for baricitinib plus remdesivir versus 7.1% (37/518) for placebo plus remdesivir.
"Baricitinib in combination with remdesivir has already provided many people with a treatment option that could help prevent progression to ventilation or death and increase recovery speed for certain hospitalized patients with COVID-19 under its currently authorized use," said Ilya Yuffa, senior vice president and president of Lilly Bio-Medicines. "Today's FDA action provides physicians additional treatment regimen options for baricitinib to continue to meet the urgent medical needs posed by this pandemic. Based on the increasing body of evidence, we are confident in the potential of baricitinib as an important treatment for the hospitalized COVID-19 patient population requiring supplemental oxygen."
"Recent clinical data have helped improve our understanding of the potential role of baricitinib in the treatment of certain hospitalized patients with COVID-19 and the broadened EUA represents a critical step in fighting the pandemic," said E. Wesley Ely, M.D., M.P.H., professor of medicine and co-director of the Critical Illness, Brain Dysfunction, and Survivorship (CIBS) Center at Vanderbilt University Medical Center and co-principal investigator of COV-BARRIER.
Related Links:
Eli Lilly and Company
Incyte
Gilead Sciences
The EUA was previously restricted to use only in combination with remdesivir and now provides for the use of baricitinib for treatment of COVID-19 in hospitalized adults and pediatric patients two years of age or older requiring supplemental oxygen, non-invasive or invasive mechanical ventilation or extracorporeal membrane oxygenation (ECMO). Baricitinib is a janus kinase inhibitor, which blocks the activity of one or more of a specific family of enzymes, interfering with the pathway that leads to inflammation. Baricitinib is a prescription oral tablet medication that is FDA-approved (and sold under the brand name Olumiant) for the treatment of moderately to severely active rheumatoid arthritis.
The FDA based its decision on data from the Phase 3 COV-BARRIER randomized, double-blind, placebo-controlled study of hospitalized patients comparing baricitinib 4 mg once daily plus standard of care versus placebo plus standard of care. Patients could remain on background standard of care, as defined per local guidelines, including antimalarials, antivirals, corticosteroids, and/or azithromycin. The most frequently used therapies were corticosteroids (79% of patients, mostly dexamethasone) and remdesivir (19% of patients). While the composite primary endpoint of COV-BARRIER, which was defined as a difference in the estimated proportion of participants progressing to non-invasive ventilation including high flow oxygen or invasive mechanical ventilation (including ECMO) or death by Day 28, did not meet statistical significance, baricitinib-treated patients (27.8%) were less likely than those receiving standard of care (30.5%) to progress to ventilation or death. A pre-specified key secondary endpoint showed baricitinib, in addition to standard of care, meaningfully reduced the risk of death by 39 percent by Day 28 when compared to standard of care alone.
The initial EUA was based on data from the Adaptive COVID-19 Treatment Trial (ACTT-2), a randomized double-blind, placebo-controlled study to evaluate the efficacy and safety of baricitinib in combination with remdesivir versus placebo with remdesivir in hospitalized patients with or without oxygen requirements conducted by the National Institute of Allergy and Infectious Diseases (NIAID), part of the National Institutes of Health (NIH). Data supporting the initial EUA included the primary endpoint of median time to recovery, which was seven days for baricitinib plus remdesivir compared to eight days for placebo plus remdesivir. Secondary endpoints included the proportion of patients who died or progressed to non-invasive ventilation/high-flow oxygen or invasive mechanical ventilation by Day 29, which was lower in baricitinib plus remdesivir (23%) compared to placebo plus remdesivir (28%), and the proportion of patients who died by Day 29 was 4.7% (24/515) for baricitinib plus remdesivir versus 7.1% (37/518) for placebo plus remdesivir.
"Baricitinib in combination with remdesivir has already provided many people with a treatment option that could help prevent progression to ventilation or death and increase recovery speed for certain hospitalized patients with COVID-19 under its currently authorized use," said Ilya Yuffa, senior vice president and president of Lilly Bio-Medicines. "Today's FDA action provides physicians additional treatment regimen options for baricitinib to continue to meet the urgent medical needs posed by this pandemic. Based on the increasing body of evidence, we are confident in the potential of baricitinib as an important treatment for the hospitalized COVID-19 patient population requiring supplemental oxygen."
"Recent clinical data have helped improve our understanding of the potential role of baricitinib in the treatment of certain hospitalized patients with COVID-19 and the broadened EUA represents a critical step in fighting the pandemic," said E. Wesley Ely, M.D., M.P.H., professor of medicine and co-director of the Critical Illness, Brain Dysfunction, and Survivorship (CIBS) Center at Vanderbilt University Medical Center and co-principal investigator of COV-BARRIER.
Related Links:
Eli Lilly and Company
Incyte
Gilead Sciences
Latest COVID-19 News
- Low-Cost System Detects SARS-CoV-2 Virus in Hospital Air Using High-Tech Bubbles
- World's First Inhalable COVID-19 Vaccine Approved in China
- COVID-19 Vaccine Patch Fights SARS-CoV-2 Variants Better than Needles
- Blood Viscosity Testing Can Predict Risk of Death in Hospitalized COVID-19 Patients
- ‘Covid Computer’ Uses AI to Detect COVID-19 from Chest CT Scans
- MRI Lung-Imaging Technique Shows Cause of Long-COVID Symptoms
- Chest CT Scans of COVID-19 Patients Could Help Distinguish Between SARS-CoV-2 Variants
- Specialized MRI Detects Lung Abnormalities in Non-Hospitalized Long COVID Patients
- AI Algorithm Identifies Hospitalized Patients at Highest Risk of Dying From COVID-19
- Sweat Sensor Detects Key Biomarkers That Provide Early Warning of COVID-19 and Flu
- Study Assesses Impact of COVID-19 on Ventilation/Perfusion Scintigraphy
- CT Imaging Study Finds Vaccination Reduces Risk of COVID-19 Associated Pulmonary Embolism
- Third Day in Hospital a ‘Tipping Point’ in Severity of COVID-19 Pneumonia
- Longer Interval Between COVID-19 Vaccines Generates Up to Nine Times as Many Antibodies
- AI Model for Monitoring COVID-19 Predicts Mortality Within First 30 Days of Admission
- AI Predicts COVID Prognosis at Near-Expert Level Based Off CT Scans
Channels
Artificial Intelligence
view channel
AI-Powered Algorithm to Revolutionize Detection of Atrial Fibrillation
Atrial fibrillation (AFib), a condition characterized by an irregular and often rapid heart rate, is linked to increased risks of stroke and heart failure. This is because the irregular heartbeat in AFib... Read more
AI Diagnostic Tool Accurately Detects Valvular Disorders Often Missed by Doctors
Doctors generally use stethoscopes to listen for the characteristic lub-dub sounds made by heart valves opening and closing. They also listen for less prominent sounds that indicate problems with these valves.... Read moreCritical Care
view channel
Stretchable Microneedles to Help In Accurate Tracking of Abnormalities and Identifying Rapid Treatment
The field of personalized medicine is transforming rapidly, with advancements like wearable devices and home testing kits making it increasingly easy to monitor a wide range of health metrics, from heart... Read more
Machine Learning Tool Identifies Rare, Undiagnosed Immune Disorders from Patient EHRs
Patients suffering from rare diseases often endure extensive delays in receiving accurate diagnoses and treatments, which can lead to unnecessary tests, worsening health, psychological strain, and significant... Read more
On-Skin Wearable Bioelectronic Device Paves Way for Intelligent Implants
A team of researchers at the University of Missouri (Columbia, MO, USA) has achieved a milestone in developing a state-of-the-art on-skin wearable bioelectronic device. This development comes from a lab... Read more
First-Of-Its-Kind Dissolvable Stent to Improve Outcomes for Patients with Severe PAD
Peripheral artery disease (PAD) affects millions and presents serious health risks, particularly its severe form, chronic limb-threatening ischemia (CLTI). CLTI develops when arteries are blocked by plaque,... Read moreSurgical Techniques
view channelHandheld Device for Fluorescence-Guided Surgery a Game Changer for Removal of High-Grade Glioma Brain Tumors
Grade III or IV gliomas are among the most common and deadly brain tumors, with around 20,000 cases annually in the U.S. and 1.2 million globally. These tumors are very aggressive and tend to infiltrate... Read more.jpg)
Cutting-Edge Robotic Bronchial Endoscopic System Provides Prompt Intervention during Emergencies
A novel robotic bronchial endoscopic system has been developed to minimize side effects and provide timely intervention for airway obstructions caused by food or foreign bodies in infants, young children,... Read morePatient Care
view channelFirst-Of-Its-Kind Portable Germicidal Light Technology Disinfects High-Touch Clinical Surfaces in Seconds
Reducing healthcare-acquired infections (HAIs) remains a pressing issue within global healthcare systems. In the United States alone, 1.7 million patients contract HAIs annually, leading to approximately... Read more
Surgical Capacity Optimization Solution Helps Hospitals Boost OR Utilization
An innovative solution has the capability to transform surgical capacity utilization by targeting the root cause of surgical block time inefficiencies. Fujitsu Limited’s (Tokyo, Japan) Surgical Capacity... Read more
Game-Changing Innovation in Surgical Instrument Sterilization Significantly Improves OR Throughput
A groundbreaking innovation enables hospitals to significantly improve instrument processing time and throughput in operating rooms (ORs) and sterile processing departments. Turbett Surgical, Inc.... Read moreHealth IT
view channel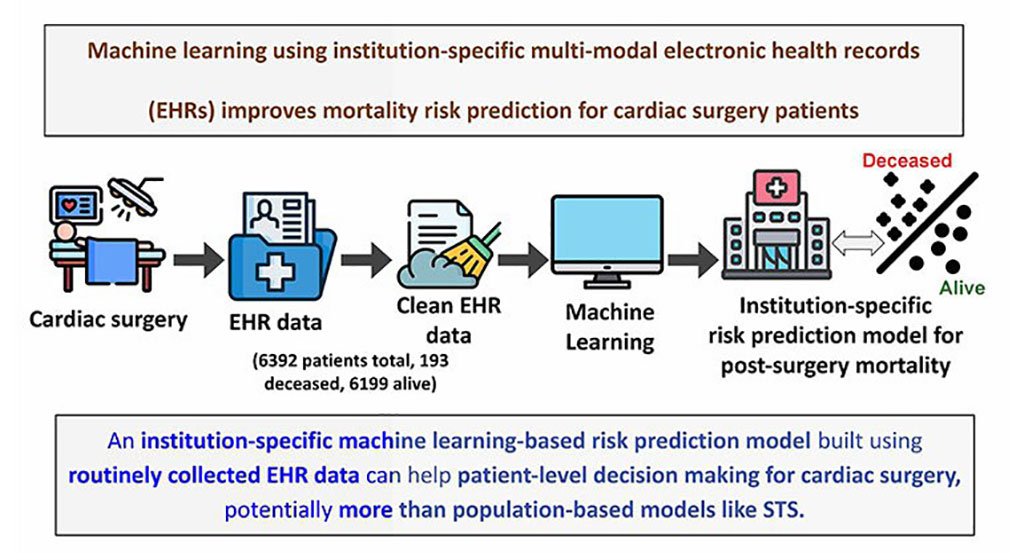
Machine Learning Model Improves Mortality Risk Prediction for Cardiac Surgery Patients
Machine learning algorithms have been deployed to create predictive models in various medical fields, with some demonstrating improved outcomes compared to their standard-of-care counterparts.... Read more
Strategic Collaboration to Develop and Integrate Generative AI into Healthcare
Top industry experts have underscored the immediate requirement for healthcare systems and hospitals to respond to severe cost and margin pressures. Close to half of U.S. hospitals ended 2022 in the red... Read more
AI-Enabled Operating Rooms Solution Helps Hospitals Maximize Utilization and Unlock Capacity
For healthcare organizations, optimizing operating room (OR) utilization during prime time hours is a complex challenge. Surgeons and clinics face difficulties in finding available slots for booking cases,... Read more
AI Predicts Pancreatic Cancer Three Years before Diagnosis from Patients’ Medical Records
Screening for common cancers like breast, cervix, and prostate cancer relies on relatively simple and highly effective techniques, such as mammograms, Pap smears, and blood tests. These methods have revolutionized... Read morePoint of Care
view channel
Critical Bleeding Management System to Help Hospitals Further Standardize Viscoelastic Testing
Surgical procedures are often accompanied by significant blood loss and the subsequent high likelihood of the need for allogeneic blood transfusions. These transfusions, while critical, are linked to various... Read more
Point of Care HIV Test Enables Early Infection Diagnosis for Infants
Early diagnosis and initiation of treatment are crucial for the survival of infants infected with HIV (human immunodeficiency virus). Without treatment, approximately 50% of infants who acquire HIV during... Read more
Whole Blood Rapid Test Aids Assessment of Concussion at Patient's Bedside
In the United States annually, approximately five million individuals seek emergency department care for traumatic brain injuries (TBIs), yet over half of those suspecting a concussion may never get it checked.... Read more
New Generation Glucose Hospital Meter System Ensures Accurate, Interference-Free and Safe Use
A new generation glucose hospital meter system now comes with several features that make hospital glucose testing easier and more secure while continuing to offer accuracy, freedom from interference, and... Read moreBusiness
view channel
Johnson & Johnson Acquires Cardiovascular Medical Device Company Shockwave Medical
Johnson & Johnson (New Brunswick, N.J., USA) and Shockwave Medical (Santa Clara, CA, USA) have entered into a definitive agreement under which Johnson & Johnson will acquire all of Shockwave’s... Read more