Architectural Design Should Promote Microbial Exposure
|
By HospiMedica International staff writers Posted on 18 Jul 2016 |
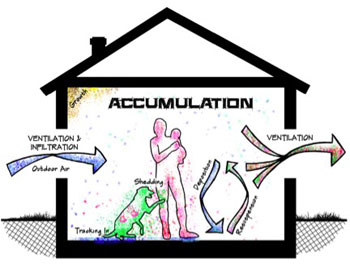
Image: Microbe accumulation in the indoor environment (Photo courtesy of Yale University).
A new study suggests that building design and operation should encourage beneficial microbial exposure, rather than focus on the disinfection of transmittable, toxic, or allergenic agents.
Researchers at Yale University (New Haven, CT, USA) sought to explore the influence that building-associated microbes have on the human microbiome. Children build a lifetime of microbial exposures through encounters with their mother's skin, breast milk, the air and surfaces in neonatal units, that first car ride home, home life and pets, daycare, and then school. And, since humans spend more than 90% of their time indoors, inhaling up to 16,000 liters of air per day, they are continuously exposed to floor and surface dust, and come into direct contact with surfaces, people, and pets.
The microbes in buildings are largely sourced from human and animal occupants and from outdoor microbes that are tracked in or enter via ventilation. They are shed from humans are dominated by skin bacteria, including high enrichments of Actinobacteria and Staphylococcaceae, and also skin-associated yeasts such as Malassezia. Pets contribute Porphyromonadaceae, Rhodocyclaceae, Pasteurellaceae, and Bacteroidetes. Due to the human-driven resuspension of dust and microbes from elevated surfaces and floors, bacterial and fungal concentrations in indoor air are often greater than those in outside air, especially in poorly ventilated buildings.
But this is not necessarily a bad thing. Growing empirical evidence links asthma protection with environmental factors known to supply a microbial exposure. In one important example, children who grow up on Bavarian or Amish farms, where homes are in close proximity to livestock, have significantly lower rates of asthma than the general, nonfarm population. This is likely because some microbes signal white blood cells to form T regulatory cells, which prevent unnecessary immune responses. Early life exposures to these microbes are important for colonizing the gut, where a significant amount of immune training occurs, playing an important role in asthma protection.
According to the researchers, the study of how building design, occupancy, and human activity impact indoor microbial communities can lead to the design of healthier buildings, and better enable studies that seek to identify the sources of beneficial and detrimental microbes. And as the identity, functions, and concentrations of beneficial microbes continue to emerge, focus must be placed on predicting how building characteristics impact building microbes, and how this ultimately shapes the human microbiome. The study was published on July 7, 2016, in Trends in Microbiology.
"One big question becomes how building design (e.g., the geographical layout, the building materials, occupancy, and ventilation) modulates microbial exposure, and our own microbiomes. As more and more beneficial microbes are identified, we--architects, engineers, and the general public--need to think about how we can facilitate our exposure to them,” said lead author Professor Jordan Peccia, PhD, of the Yale department of chemical and environmental engineering. “We can work to develop new, quantitative approaches for solving these problems--something better than our portable air filters and inhalers.”
Related Links:
Yale University
Researchers at Yale University (New Haven, CT, USA) sought to explore the influence that building-associated microbes have on the human microbiome. Children build a lifetime of microbial exposures through encounters with their mother's skin, breast milk, the air and surfaces in neonatal units, that first car ride home, home life and pets, daycare, and then school. And, since humans spend more than 90% of their time indoors, inhaling up to 16,000 liters of air per day, they are continuously exposed to floor and surface dust, and come into direct contact with surfaces, people, and pets.
The microbes in buildings are largely sourced from human and animal occupants and from outdoor microbes that are tracked in or enter via ventilation. They are shed from humans are dominated by skin bacteria, including high enrichments of Actinobacteria and Staphylococcaceae, and also skin-associated yeasts such as Malassezia. Pets contribute Porphyromonadaceae, Rhodocyclaceae, Pasteurellaceae, and Bacteroidetes. Due to the human-driven resuspension of dust and microbes from elevated surfaces and floors, bacterial and fungal concentrations in indoor air are often greater than those in outside air, especially in poorly ventilated buildings.
But this is not necessarily a bad thing. Growing empirical evidence links asthma protection with environmental factors known to supply a microbial exposure. In one important example, children who grow up on Bavarian or Amish farms, where homes are in close proximity to livestock, have significantly lower rates of asthma than the general, nonfarm population. This is likely because some microbes signal white blood cells to form T regulatory cells, which prevent unnecessary immune responses. Early life exposures to these microbes are important for colonizing the gut, where a significant amount of immune training occurs, playing an important role in asthma protection.
According to the researchers, the study of how building design, occupancy, and human activity impact indoor microbial communities can lead to the design of healthier buildings, and better enable studies that seek to identify the sources of beneficial and detrimental microbes. And as the identity, functions, and concentrations of beneficial microbes continue to emerge, focus must be placed on predicting how building characteristics impact building microbes, and how this ultimately shapes the human microbiome. The study was published on July 7, 2016, in Trends in Microbiology.
"One big question becomes how building design (e.g., the geographical layout, the building materials, occupancy, and ventilation) modulates microbial exposure, and our own microbiomes. As more and more beneficial microbes are identified, we--architects, engineers, and the general public--need to think about how we can facilitate our exposure to them,” said lead author Professor Jordan Peccia, PhD, of the Yale department of chemical and environmental engineering. “We can work to develop new, quantitative approaches for solving these problems--something better than our portable air filters and inhalers.”
Related Links:
Yale University
Latest Hospital News News
- Nurse Tracking System Improves Hospital Workflow
- New Children’s Hospital Transforms California Healthcare
- Noisy Hospitals Face Threat of Decreased Federal Compensation
- Orthopedics Centre of Excellence Planned for Guy’s Hospital
- Research Suggests Avoidance of Low-Value Surgical Procedures
- U.S. Federal Readmission Fines Linked to Higher Mortality
- Columbia China to Build New Hospital in Jiaxing
- Dubai Debuts Second Robotic Pharmacy Service
- Seattle Hospital Network Shifts Away from Overlapping Surgeries
- ACC to Launch Valvular Heart Disease Program in China
- Mortality Rates Lower at Major Teaching Hospitals
- South Australia to Inaugurate Upscale Hospital
- Raffles to Launch Second Hospital Project in China
- Research Center Tackles Antimicrobial Drugs Challenge
- Miami Cardiac & Vascular Institute Completes Expansion Project
- Hospital Antibiotic Policies Improve Prescription Practices
Channels
Artificial Intelligence
view channel
AI-Powered Algorithm to Revolutionize Detection of Atrial Fibrillation
Atrial fibrillation (AFib), a condition characterized by an irregular and often rapid heart rate, is linked to increased risks of stroke and heart failure. This is because the irregular heartbeat in AFib... Read more
AI Diagnostic Tool Accurately Detects Valvular Disorders Often Missed by Doctors
Doctors generally use stethoscopes to listen for the characteristic lub-dub sounds made by heart valves opening and closing. They also listen for less prominent sounds that indicate problems with these valves.... Read moreCritical Care
view channel
Stretchable Microneedles to Help In Accurate Tracking of Abnormalities and Identifying Rapid Treatment
The field of personalized medicine is transforming rapidly, with advancements like wearable devices and home testing kits making it increasingly easy to monitor a wide range of health metrics, from heart... Read more
Machine Learning Tool Identifies Rare, Undiagnosed Immune Disorders from Patient EHRs
Patients suffering from rare diseases often endure extensive delays in receiving accurate diagnoses and treatments, which can lead to unnecessary tests, worsening health, psychological strain, and significant... Read more
On-Skin Wearable Bioelectronic Device Paves Way for Intelligent Implants
A team of researchers at the University of Missouri (Columbia, MO, USA) has achieved a milestone in developing a state-of-the-art on-skin wearable bioelectronic device. This development comes from a lab... Read more
First-Of-Its-Kind Dissolvable Stent to Improve Outcomes for Patients with Severe PAD
Peripheral artery disease (PAD) affects millions and presents serious health risks, particularly its severe form, chronic limb-threatening ischemia (CLTI). CLTI develops when arteries are blocked by plaque,... Read moreSurgical Techniques
view channel
Small, Implantable Cardiac Pump to Help Children Awaiting Heart Transplant
Implantable ventricular assist devices, available for adults for over 40 years, fit inside the chest and are generally safer and easier to use than external devices. These devices enable patients to live... Read moreGastrointestinal Imaging Capsule a Game-Changer in Esophagus Surveillance and Treatment
A newly-developed gastrointestinal imaging capsule is poised to be a game-changer in esophagus surveillance and interventions. The Multifunctional Ablative Gastrointestinal Imaging Capsule (MAGIC) developed... Read more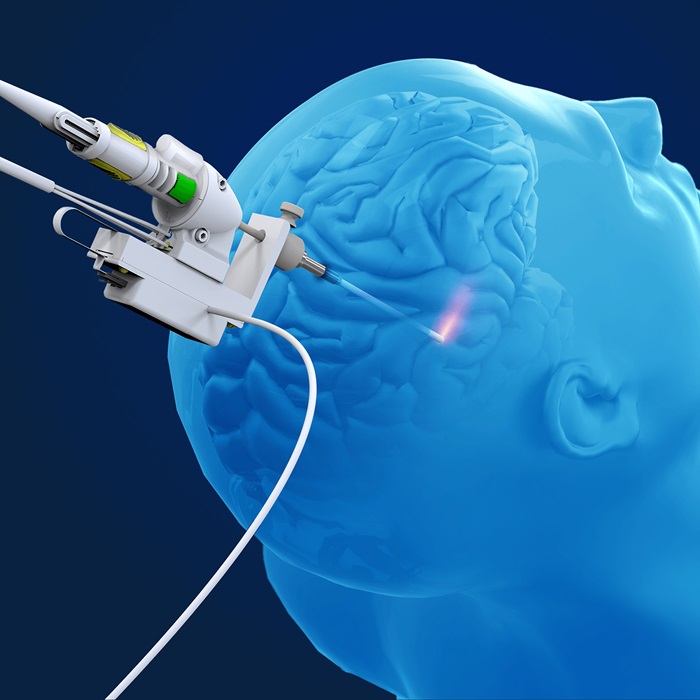
World’s Smallest Laser Probe for Brain Procedures Facilitates Ablation of Full Range of Targets
A new probe enhances the ablation capabilities for a broad spectrum of oncology and epilepsy targets, including pediatric applications, by incorporating advanced laser and cooling technologies to support... Read more.jpg)
Artificial Intelligence Broadens Diagnostic Abilities of Conventional Coronary Angiography
Coronary angiography is an essential diagnostic tool used globally to identify coronary artery disease (CAD), with millions of procedures conducted annually. Traditionally, data from coronary angiograms... Read morePatient Care
view channelFirst-Of-Its-Kind Portable Germicidal Light Technology Disinfects High-Touch Clinical Surfaces in Seconds
Reducing healthcare-acquired infections (HAIs) remains a pressing issue within global healthcare systems. In the United States alone, 1.7 million patients contract HAIs annually, leading to approximately... Read more
Surgical Capacity Optimization Solution Helps Hospitals Boost OR Utilization
An innovative solution has the capability to transform surgical capacity utilization by targeting the root cause of surgical block time inefficiencies. Fujitsu Limited’s (Tokyo, Japan) Surgical Capacity... Read more
Game-Changing Innovation in Surgical Instrument Sterilization Significantly Improves OR Throughput
A groundbreaking innovation enables hospitals to significantly improve instrument processing time and throughput in operating rooms (ORs) and sterile processing departments. Turbett Surgical, Inc.... Read moreHealth IT
view channel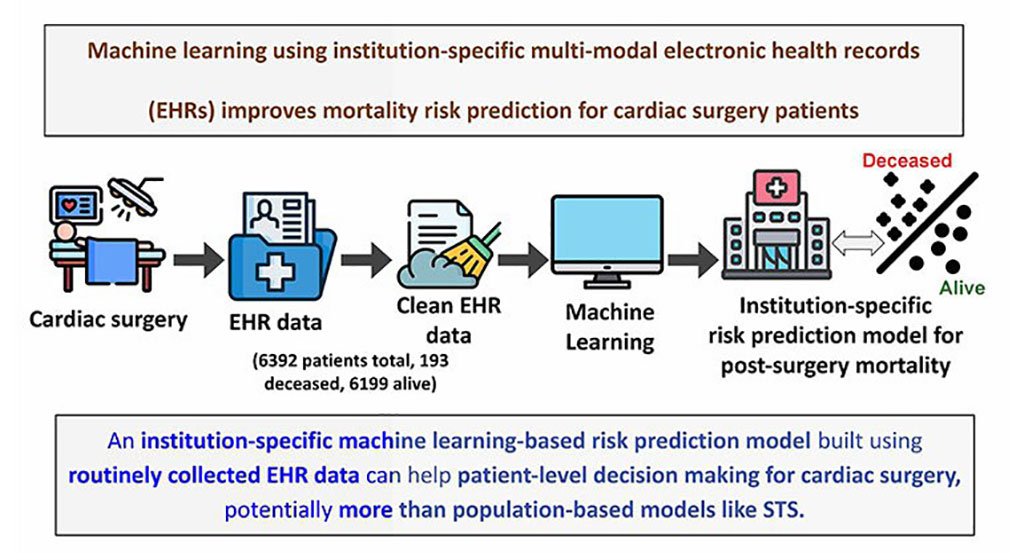
Machine Learning Model Improves Mortality Risk Prediction for Cardiac Surgery Patients
Machine learning algorithms have been deployed to create predictive models in various medical fields, with some demonstrating improved outcomes compared to their standard-of-care counterparts.... Read more
Strategic Collaboration to Develop and Integrate Generative AI into Healthcare
Top industry experts have underscored the immediate requirement for healthcare systems and hospitals to respond to severe cost and margin pressures. Close to half of U.S. hospitals ended 2022 in the red... Read more
AI-Enabled Operating Rooms Solution Helps Hospitals Maximize Utilization and Unlock Capacity
For healthcare organizations, optimizing operating room (OR) utilization during prime time hours is a complex challenge. Surgeons and clinics face difficulties in finding available slots for booking cases,... Read more
AI Predicts Pancreatic Cancer Three Years before Diagnosis from Patients’ Medical Records
Screening for common cancers like breast, cervix, and prostate cancer relies on relatively simple and highly effective techniques, such as mammograms, Pap smears, and blood tests. These methods have revolutionized... Read morePoint of Care
view channel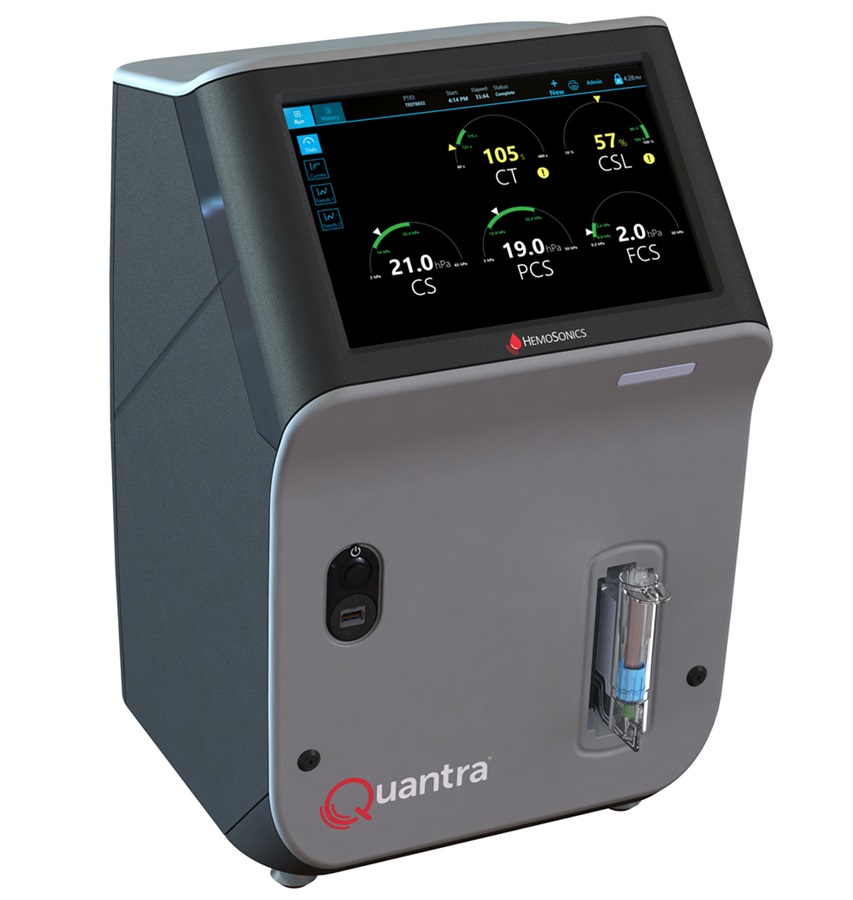
Critical Bleeding Management System to Help Hospitals Further Standardize Viscoelastic Testing
Surgical procedures are often accompanied by significant blood loss and the subsequent high likelihood of the need for allogeneic blood transfusions. These transfusions, while critical, are linked to various... Read more
Point of Care HIV Test Enables Early Infection Diagnosis for Infants
Early diagnosis and initiation of treatment are crucial for the survival of infants infected with HIV (human immunodeficiency virus). Without treatment, approximately 50% of infants who acquire HIV during... Read more
Whole Blood Rapid Test Aids Assessment of Concussion at Patient's Bedside
In the United States annually, approximately five million individuals seek emergency department care for traumatic brain injuries (TBIs), yet over half of those suspecting a concussion may never get it checked.... Read more
New Generation Glucose Hospital Meter System Ensures Accurate, Interference-Free and Safe Use
A new generation glucose hospital meter system now comes with several features that make hospital glucose testing easier and more secure while continuing to offer accuracy, freedom from interference, and... Read moreBusiness
view channel
Johnson & Johnson Acquires Cardiovascular Medical Device Company Shockwave Medical
Johnson & Johnson (New Brunswick, N.J., USA) and Shockwave Medical (Santa Clara, CA, USA) have entered into a definitive agreement under which Johnson & Johnson will acquire all of Shockwave’s... Read more