Hospital Antibiotic Policies Improve Prescription Practices
|
By HospiMedica International staff writers Posted on 21 Feb 2017 |
An updated review of studies identifies effective guidelines and policies to reduce unnecessary use of antibiotics in hospitals.
Researchers at the University of Dundee, University College London, and other institutions searched the Cochrane Central Register of Controlled Trials (CENTRAL), MEDLINE, and Embase for studies examining the effectiveness and safety of interventions designed to improve antibiotic prescribing to hospital inpatients, and to investigate the effect of different intervention functions. In all, the researchers found 221 studies from the United States, Europe, Asia, South America, and Australia.
The researchers found that interventions broadly fell into two categories; 'restrictive' techniques applied rules to make physicians prescribe properly, whilst 'enabling' techniques provided advice or feedback to help physicians make more informed prescribing decisions. In both cases, the aim of the intervention was to increase the number of appropriate prescribing decisions so that patients who were unlikely to benefit from antibiotics did not get them, whilst they were still used for patients who stood to benefit from them.
The results showed that interventions that included enabling or restrictive techniques were consistently more effective than interventions that relied on simple education alone. Moreover, a synergistic effect existed, with enabling techniques increasing the effectiveness of restrictive techniques. In addition, the interventions shortened duration of antibiotic use from 11 to 9 days per patient, and reduced hospital stay from an average of 13 days to 12 per patient. The review was published on February 9, 2017, in The Cochrane Library.
“We do not need more studies to answer the question of whether these interventions reduce unnecessary antibiotic use, but we do need more research to understand why the most effective behavior change techniques are not more widely adopted within hospital settings,” concluded lead author Peter Davey, PhD, of the UD department of population health sciences. “Appropriate antibiotic use in hospitals should ensure effective treatment of patients with infection, and reduce unnecessary prescriptions.”
For the study, the researchers defined restriction as using rules to reduce the opportunity to engage in the target behavior, or increase the target behavior by reducing the opportunity to engage in competing behaviors. Enablement was defined as increasing the means and reducing the barriers in order to increase capability or opportunity.
Researchers at the University of Dundee, University College London, and other institutions searched the Cochrane Central Register of Controlled Trials (CENTRAL), MEDLINE, and Embase for studies examining the effectiveness and safety of interventions designed to improve antibiotic prescribing to hospital inpatients, and to investigate the effect of different intervention functions. In all, the researchers found 221 studies from the United States, Europe, Asia, South America, and Australia.
The researchers found that interventions broadly fell into two categories; 'restrictive' techniques applied rules to make physicians prescribe properly, whilst 'enabling' techniques provided advice or feedback to help physicians make more informed prescribing decisions. In both cases, the aim of the intervention was to increase the number of appropriate prescribing decisions so that patients who were unlikely to benefit from antibiotics did not get them, whilst they were still used for patients who stood to benefit from them.
The results showed that interventions that included enabling or restrictive techniques were consistently more effective than interventions that relied on simple education alone. Moreover, a synergistic effect existed, with enabling techniques increasing the effectiveness of restrictive techniques. In addition, the interventions shortened duration of antibiotic use from 11 to 9 days per patient, and reduced hospital stay from an average of 13 days to 12 per patient. The review was published on February 9, 2017, in The Cochrane Library.
“We do not need more studies to answer the question of whether these interventions reduce unnecessary antibiotic use, but we do need more research to understand why the most effective behavior change techniques are not more widely adopted within hospital settings,” concluded lead author Peter Davey, PhD, of the UD department of population health sciences. “Appropriate antibiotic use in hospitals should ensure effective treatment of patients with infection, and reduce unnecessary prescriptions.”
For the study, the researchers defined restriction as using rules to reduce the opportunity to engage in the target behavior, or increase the target behavior by reducing the opportunity to engage in competing behaviors. Enablement was defined as increasing the means and reducing the barriers in order to increase capability or opportunity.
Latest Hospital News News
- Nurse Tracking System Improves Hospital Workflow
- New Children’s Hospital Transforms California Healthcare
- Noisy Hospitals Face Threat of Decreased Federal Compensation
- Orthopedics Centre of Excellence Planned for Guy’s Hospital
- Research Suggests Avoidance of Low-Value Surgical Procedures
- U.S. Federal Readmission Fines Linked to Higher Mortality
- Columbia China to Build New Hospital in Jiaxing
- Dubai Debuts Second Robotic Pharmacy Service
- Seattle Hospital Network Shifts Away from Overlapping Surgeries
- ACC to Launch Valvular Heart Disease Program in China
- Mortality Rates Lower at Major Teaching Hospitals
- South Australia to Inaugurate Upscale Hospital
- Raffles to Launch Second Hospital Project in China
- Research Center Tackles Antimicrobial Drugs Challenge
- Miami Cardiac & Vascular Institute Completes Expansion Project
- USC Virtual Care Clinic to Employ Avatar Doctors
Channels
Artificial Intelligence
view channel
AI-Powered Algorithm to Revolutionize Detection of Atrial Fibrillation
Atrial fibrillation (AFib), a condition characterized by an irregular and often rapid heart rate, is linked to increased risks of stroke and heart failure. This is because the irregular heartbeat in AFib... Read more
AI Diagnostic Tool Accurately Detects Valvular Disorders Often Missed by Doctors
Doctors generally use stethoscopes to listen for the characteristic lub-dub sounds made by heart valves opening and closing. They also listen for less prominent sounds that indicate problems with these valves.... Read moreCritical Care
view channel
AI Brain-Age Estimation Technology Uses EEG Scans to Screen for Degenerative Diseases
As individuals age, so do their brains. Premature aging of the brain can lead to age-related conditions such as mild cognitive impairment, dementia, or Parkinson's disease. The ability to determine "brain... Read more
Wheeze-Counting Wearable Device Monitors Patient's Breathing In Real Time
Lung diseases like asthma, chronic obstructive pulmonary disease (COPD), lung cancer, bronchitis, and infections such as pneumonia, rank among the leading causes of death worldwide. Traditionally, medical... Read moreSurgical Techniques
view channel
Robotic Nerve ‘Cuffs’ Could Treat Various Neurological Conditions
Electric nerve implants serve dual functions: they can either stimulate or block signals in specific nerves. For example, they may alleviate pain by inhibiting pain signals or restore movement in paralyzed... Read more
Flexible Microdisplay Visualizes Brain Activity in Real-Time To Guide Neurosurgeons
During brain surgery, neurosurgeons need to identify and preserve regions responsible for critical functions while removing harmful tissue. Traditionally, neurosurgeons rely on a team of electrophysiologists,... Read more.jpg)
Next-Gen Computer Assisted Vacuum Thrombectomy Technology Rapidly Removes Blood Clots
Pulmonary embolism (PE) occurs when a blood clot blocks one of the arteries in the lungs. Often, these clots originate from the leg or another part of the body, a condition known as deep vein thrombosis,... Read morePatient Care
view channel
Surgical Capacity Optimization Solution Helps Hospitals Boost OR Utilization
An innovative solution has the capability to transform surgical capacity utilization by targeting the root cause of surgical block time inefficiencies. Fujitsu Limited’s (Tokyo, Japan) Surgical Capacity... Read more
Game-Changing Innovation in Surgical Instrument Sterilization Significantly Improves OR Throughput
A groundbreaking innovation enables hospitals to significantly improve instrument processing time and throughput in operating rooms (ORs) and sterile processing departments. Turbett Surgical, Inc.... Read more
Next Gen ICU Bed to Help Address Complex Critical Care Needs
As the critical care environment becomes increasingly demanding and complex due to evolving hospital needs, there is a pressing requirement for innovations that can facilitate patient recovery.... Read moreGroundbreaking AI-Powered UV-C Disinfection Technology Redefines Infection Control Landscape
Healthcare-associated infection (HCAI) is a widespread complication in healthcare management, posing a significant health risk due to its potential to increase patient morbidity and mortality, prolong... Read moreHealth IT
view channel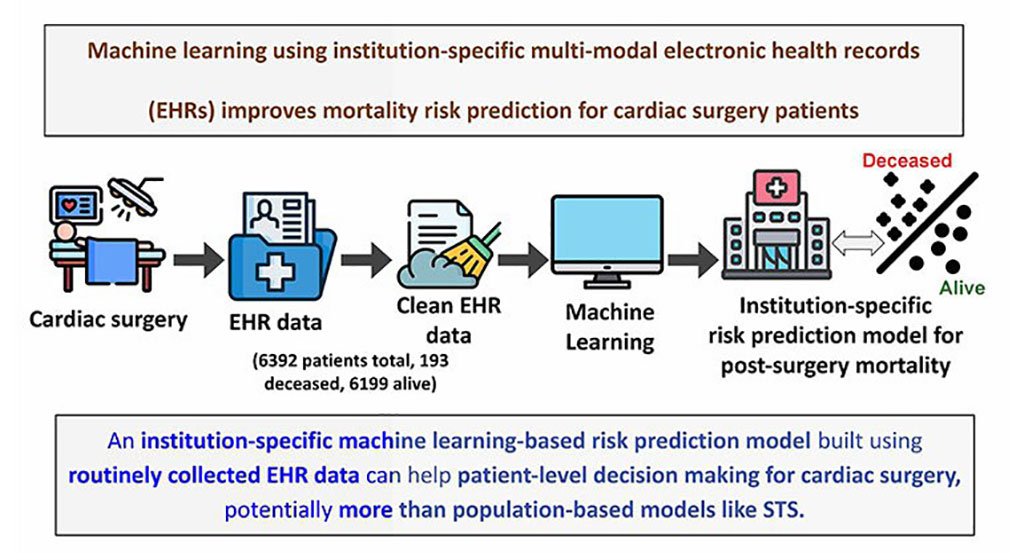
Machine Learning Model Improves Mortality Risk Prediction for Cardiac Surgery Patients
Machine learning algorithms have been deployed to create predictive models in various medical fields, with some demonstrating improved outcomes compared to their standard-of-care counterparts.... Read more
Strategic Collaboration to Develop and Integrate Generative AI into Healthcare
Top industry experts have underscored the immediate requirement for healthcare systems and hospitals to respond to severe cost and margin pressures. Close to half of U.S. hospitals ended 2022 in the red... Read more
AI-Enabled Operating Rooms Solution Helps Hospitals Maximize Utilization and Unlock Capacity
For healthcare organizations, optimizing operating room (OR) utilization during prime time hours is a complex challenge. Surgeons and clinics face difficulties in finding available slots for booking cases,... Read more
AI Predicts Pancreatic Cancer Three Years before Diagnosis from Patients’ Medical Records
Screening for common cancers like breast, cervix, and prostate cancer relies on relatively simple and highly effective techniques, such as mammograms, Pap smears, and blood tests. These methods have revolutionized... Read morePoint of Care
view channel
Critical Bleeding Management System to Help Hospitals Further Standardize Viscoelastic Testing
Surgical procedures are often accompanied by significant blood loss and the subsequent high likelihood of the need for allogeneic blood transfusions. These transfusions, while critical, are linked to various... Read more
Point of Care HIV Test Enables Early Infection Diagnosis for Infants
Early diagnosis and initiation of treatment are crucial for the survival of infants infected with HIV (human immunodeficiency virus). Without treatment, approximately 50% of infants who acquire HIV during... Read more
Whole Blood Rapid Test Aids Assessment of Concussion at Patient's Bedside
In the United States annually, approximately five million individuals seek emergency department care for traumatic brain injuries (TBIs), yet over half of those suspecting a concussion may never get it checked.... Read more
New Generation Glucose Hospital Meter System Ensures Accurate, Interference-Free and Safe Use
A new generation glucose hospital meter system now comes with several features that make hospital glucose testing easier and more secure while continuing to offer accuracy, freedom from interference, and... Read moreBusiness
view channel
Johnson & Johnson Acquires Cardiovascular Medical Device Company Shockwave Medical
Johnson & Johnson (New Brunswick, N.J., USA) and Shockwave Medical (Santa Clara, CA, USA) have entered into a definitive agreement under which Johnson & Johnson will acquire all of Shockwave’s... Read more