Flushing Fallopian Tubes Moderates Infertility
|
By HospiMedica International staff writers Posted on 01 Jun 2017 |
Image: A new study suggests an old imaging technique can give new hope as an infertility treatment (Photo courtesy of MNT).
A new study suggests that hysterosalpingography (HSG), a century-old fluoroscopic imaging technique, can dramatically reduce infertility rates.
Researchers at the University of Adelaide, VU University Medical Centre, and other institutions conducted a multicenter, randomized trial in 27 hospitals in the Netherlands in which 1,119 infertile women undergoing HSG were randomly assigned to either an oil-based or water-based contrast agent. The couples then underwent expectant management, or the women underwent intrauterine insemination. The primary outcome was ongoing pregnancy within six months of randomization.
In all, 557 women were assigned to HSG using oil contrast, and 562 women were assigned to water contrast. After six months, 39.7% of the women in the oil group and 29.1% women in the water group had an ongoing pregnancy. At the termination of the study, 38.8% of women in the oil group and 28.1% of women in the water group had live births. Rates of adverse events were low and similar in the two groups. The study was presented at the 13th World Congress on Endometriosis, held during May 2017 in Vancouver (Canada).
“Over the past century, pregnancy rates among infertile women reportedly increased after their tubes had been flushed with either water or oil during this X-ray procedure. Until now, it has been unclear whether the type of solution used in the procedure was influencing the change in fertility,” said senior author Professor Ben Mol, MD, PhD, who was conceived after his mother underwent HSG. “Our results have been even more exciting than we could have predicted, helping to confirm that an age-old medical technique still has an important place in modern medicine.”
HSG is an x-ray fluoroscopy technique to examine the uterus and fallopian tubes of a woman who is having difficulty becoming pregnant. First carried out in 1917, the procedure is also used to investigate miscarriages and to determine presence and severity of tumor masses, adhesions, and uterine fibroids. The underlying mechanisms by which HSG might enhance fertility are unclear; some studies suggest that it flushes debris and dislodge mucus plugs from undamaged tubes. The oil contrast might also have an effect on peritoneal macrophage activity and on endometrial receptivity, thereby enhancing fertility by an implantation-mediated mechanism.
Researchers at the University of Adelaide, VU University Medical Centre, and other institutions conducted a multicenter, randomized trial in 27 hospitals in the Netherlands in which 1,119 infertile women undergoing HSG were randomly assigned to either an oil-based or water-based contrast agent. The couples then underwent expectant management, or the women underwent intrauterine insemination. The primary outcome was ongoing pregnancy within six months of randomization.
In all, 557 women were assigned to HSG using oil contrast, and 562 women were assigned to water contrast. After six months, 39.7% of the women in the oil group and 29.1% women in the water group had an ongoing pregnancy. At the termination of the study, 38.8% of women in the oil group and 28.1% of women in the water group had live births. Rates of adverse events were low and similar in the two groups. The study was presented at the 13th World Congress on Endometriosis, held during May 2017 in Vancouver (Canada).
“Over the past century, pregnancy rates among infertile women reportedly increased after their tubes had been flushed with either water or oil during this X-ray procedure. Until now, it has been unclear whether the type of solution used in the procedure was influencing the change in fertility,” said senior author Professor Ben Mol, MD, PhD, who was conceived after his mother underwent HSG. “Our results have been even more exciting than we could have predicted, helping to confirm that an age-old medical technique still has an important place in modern medicine.”
HSG is an x-ray fluoroscopy technique to examine the uterus and fallopian tubes of a woman who is having difficulty becoming pregnant. First carried out in 1917, the procedure is also used to investigate miscarriages and to determine presence and severity of tumor masses, adhesions, and uterine fibroids. The underlying mechanisms by which HSG might enhance fertility are unclear; some studies suggest that it flushes debris and dislodge mucus plugs from undamaged tubes. The oil contrast might also have an effect on peritoneal macrophage activity and on endometrial receptivity, thereby enhancing fertility by an implantation-mediated mechanism.
Latest Patient Care News
- Surgical Capacity Optimization Solution Helps Hospitals Boost OR Utilization

- Game-Changing Innovation in Surgical Instrument Sterilization Significantly Improves OR Throughput
- Next Gen ICU Bed to Help Address Complex Critical Care Needs
- Groundbreaking AI-Powered UV-C Disinfection Technology Redefines Infection Control Landscape
- Clean Hospitals Can Reduce Antibiotic Resistance, Save Lives
- Smart Hospital Beds Improve Accuracy of Medical Diagnosis
- New Fast Endoscope Drying System Improves Productivity and Traceability
- World’s First Automated Endoscope Cleaner Fights Antimicrobial Resistance
- Portable High-Capacity Digital Stretcher Scales Provide Precision Weighing for Patients in ER
- Portable Clinical Scale with Remote Indicator Allows for Flexible Patient Weighing Use
- Innovative and Highly Customizable Medical Carts Offer Unlimited Configuration Possibilities
- Biomolecular Wound Healing Film Adheres to Sensitive Tissue and Releases Active Ingredients
- Wearable Health Tech Could Measure Gases Released From Skin to Monitor Metabolic Diseases
- Wearable Cardioverter Defibrillator System Protects Patients at Risk of Sudden Cardiac Arrest
- World's First AI-Ready Infrasound Stethoscope Listens to Bodily Sounds Not Audible to Human Ear
- POC Diagnostic Platform Offers Handheld, Instrument-Free PCR Testing for STIs
Channels
Artificial Intelligence
view channel
AI-Powered Algorithm to Revolutionize Detection of Atrial Fibrillation
Atrial fibrillation (AFib), a condition characterized by an irregular and often rapid heart rate, is linked to increased risks of stroke and heart failure. This is because the irregular heartbeat in AFib... Read more
AI Diagnostic Tool Accurately Detects Valvular Disorders Often Missed by Doctors
Doctors generally use stethoscopes to listen for the characteristic lub-dub sounds made by heart valves opening and closing. They also listen for less prominent sounds that indicate problems with these valves.... Read moreCritical Care
view channel
Wheeze-Counting Wearable Device Monitors Patient's Breathing In Real Time
Lung diseases like asthma, chronic obstructive pulmonary disease (COPD), lung cancer, bronchitis, and infections such as pneumonia, rank among the leading causes of death worldwide. Traditionally, medical... Read more
Wearable Multiplex Biosensors Could Revolutionize COPD Management
Chronic obstructive pulmonary disease (COPD) ranks as the third leading cause of death worldwide. Acute exacerbations of COPD (AECOPD), which are often triggered by lung infections, accelerate the disease's... Read moreSurgical Techniques
view channel
Flexible Microdisplay Visualizes Brain Activity in Real-Time To Guide Neurosurgeons
During brain surgery, neurosurgeons need to identify and preserve regions responsible for critical functions while removing harmful tissue. Traditionally, neurosurgeons rely on a team of electrophysiologists,... Read more.jpg)
Next-Gen Computer Assisted Vacuum Thrombectomy Technology Rapidly Removes Blood Clots
Pulmonary embolism (PE) occurs when a blood clot blocks one of the arteries in the lungs. Often, these clots originate from the leg or another part of the body, a condition known as deep vein thrombosis,... Read more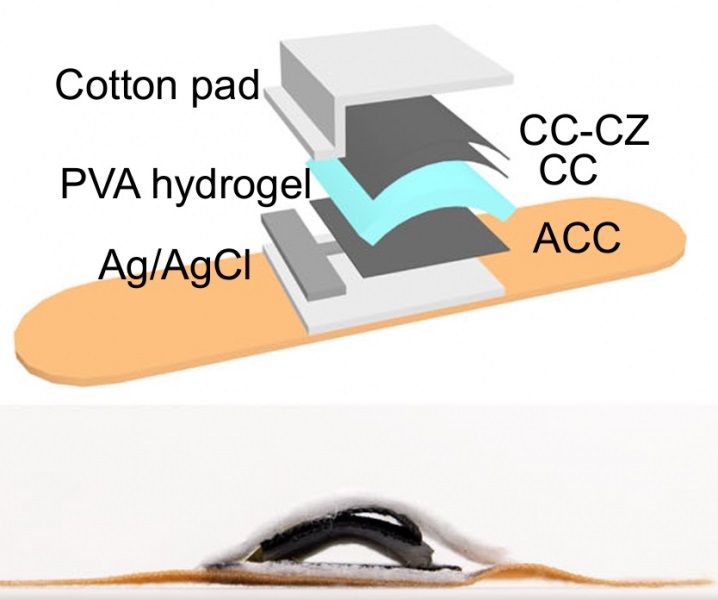
Hydrogel-Based Miniaturized Electric Generators to Power Biomedical Devices
The development of engineered devices that can harvest and convert the mechanical motion of the human body into electricity is essential for powering bioelectronic devices. This mechanoelectrical energy... Read moreWearable Technology Monitors and Analyzes Surgeons' Posture during Long Surgical Procedures
The physical strain associated with the static postures maintained by neurosurgeons during long operations can lead to fatigue and musculoskeletal problems. An objective assessment of surgical ergonomics... Read moreHealth IT
view channel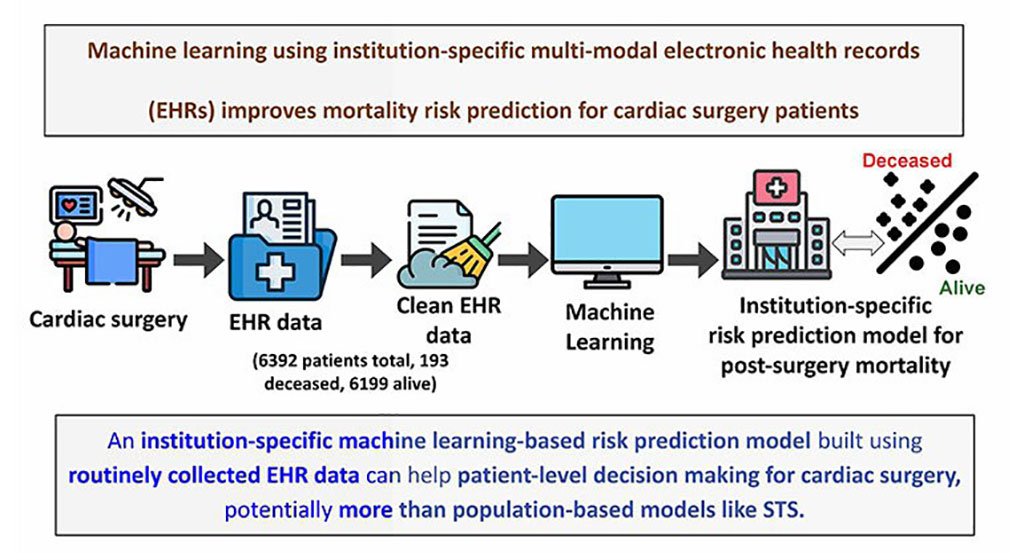
Machine Learning Model Improves Mortality Risk Prediction for Cardiac Surgery Patients
Machine learning algorithms have been deployed to create predictive models in various medical fields, with some demonstrating improved outcomes compared to their standard-of-care counterparts.... Read more
Strategic Collaboration to Develop and Integrate Generative AI into Healthcare
Top industry experts have underscored the immediate requirement for healthcare systems and hospitals to respond to severe cost and margin pressures. Close to half of U.S. hospitals ended 2022 in the red... Read more
AI-Enabled Operating Rooms Solution Helps Hospitals Maximize Utilization and Unlock Capacity
For healthcare organizations, optimizing operating room (OR) utilization during prime time hours is a complex challenge. Surgeons and clinics face difficulties in finding available slots for booking cases,... Read more
AI Predicts Pancreatic Cancer Three Years before Diagnosis from Patients’ Medical Records
Screening for common cancers like breast, cervix, and prostate cancer relies on relatively simple and highly effective techniques, such as mammograms, Pap smears, and blood tests. These methods have revolutionized... Read morePoint of Care
view channel
Critical Bleeding Management System to Help Hospitals Further Standardize Viscoelastic Testing
Surgical procedures are often accompanied by significant blood loss and the subsequent high likelihood of the need for allogeneic blood transfusions. These transfusions, while critical, are linked to various... Read more
Point of Care HIV Test Enables Early Infection Diagnosis for Infants
Early diagnosis and initiation of treatment are crucial for the survival of infants infected with HIV (human immunodeficiency virus). Without treatment, approximately 50% of infants who acquire HIV during... Read more
Whole Blood Rapid Test Aids Assessment of Concussion at Patient's Bedside
In the United States annually, approximately five million individuals seek emergency department care for traumatic brain injuries (TBIs), yet over half of those suspecting a concussion may never get it checked.... Read more
New Generation Glucose Hospital Meter System Ensures Accurate, Interference-Free and Safe Use
A new generation glucose hospital meter system now comes with several features that make hospital glucose testing easier and more secure while continuing to offer accuracy, freedom from interference, and... Read moreBusiness
view channel
Johnson & Johnson Acquires Cardiovascular Medical Device Company Shockwave Medical
Johnson & Johnson (New Brunswick, N.J., USA) and Shockwave Medical (Santa Clara, CA, USA) have entered into a definitive agreement under which Johnson & Johnson will acquire all of Shockwave’s... Read more












.jpg)
